CLEMENTE RONCHETTA
FRANCESCO BOCCUZZI
DEFINITION
Thalassemia (from Greek θαλασσα, thalassa, sea + αίμα, haima, blood) is an inherited autosomal recessive blood disease. In thalassemia, the genetic defect results in reduced rate of synthesis of one of the globin chains that make up hemoglobin. Reduced synthesis of one of the globin chains can cause the formation of abnormal hemoglobin molecules, and this in turn causes the anemia which is the characteristic presenting symptom of the thalassemias.
EPIDEMIOLOGY
The most prevalent genetic disorder in the world with an high prevalence in a belt around the earth, which is around the 40th parallel in the Mediterranean area but eastwards moves further south, reaching the equator in Indonesia. It is rare in people of Northern European origin, around 1: 1000 are carriers, while in the Northern Mediterranean countries (S. Europe) the carrier prevalence is 1-19%.

Italy represents a small group of high prevalence Mediterranean countries, which have developed control programs (treatment and prevention) within the context of a developed health provision system.
This north-south divide has been gradually changing: the factors affecting epidemiological change in genetic disease have been recognized as selection, genetic drift and migrations.

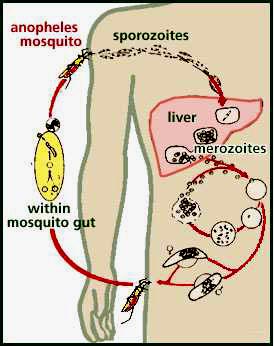
Selective advantage of the carrier state of the Thalassemias and haemoglobinopathies by increased resistance to Malaria. has been proposed as the reason for their high prevalence in these areas.

SYMPTOMS
Clinical severity varies widely, depending on the degree to wich the synthesis of the affected globin is imparied, altered synthesis of other chains, and co-inheritance of other abnormal globin alleles.
In heterozygotes (β-Thalassemia Trait)
- hypochromia and mycrocitosis
- anemia is minimal

In more severe homozygous states (β-Thalassemia Mayor or Cooley's Anemia) there is accumulation of higly insoluble umpaired alpha chains, they form toxic inclusion bodies that kill developing erytrhoblasts in the marrow and shorten RBC life span leading to
** severe hemolytic anemia
** pale and listless appearance
** poor appetite
** dark urine
** slowed growth and delayed puberty
** jaundice, leg ulcers and gallstones
** enlarged spleen, liver (due to masses of extramedullary erythropoietic tissue)
** bone problems (massive bone marrow expansion)
** high output congestive heart failure

β-Thalassemia Trait:
Hemoglobin, Hematocrit are decreased, the RBC count is not as low as the hemoglobin and hematocrit, in fact it is usually normal. Indecies show a characteristic discordance: the MCV is slightly decreased and the MCH is decreased, the MCHC is normal.
Morphology is microcytic and hypochromic. Anisocytosis is only slight and not near as marked as in iron deficiency.
Bone marrow: normal to slight erythroid hyperplasia.
Tests for iron deficiency: normal
Bilirubin: slight increase due to intramedullary hemolysis
Hemoglobin studies:
* Hgb A decreased,
* Hgb A2 increased,
* Hgb F increase to normal

β-Thalassemia Mayor:
Anemia is severe: Hgb 20 to 30 g/L. Hematocrit and RBC count are also decreased hence the indecies MCV, MCH and MCHC are all decreased, the RDW is increased.
The morphology is severe hypochromic microcytic with marked aniso and poik.
Bone marrow - erythroid hyperplasia with dyserythropoiesis.
Tests for iron deficiency:
* Stainable - increased and a rare ringed sideroblast may be seen.
* Serum iron - increased/normal
* Ferritin - increased/normal
* %saturation - increased
Hemoglobin electrophoresis:
* Hgb A decreased,
* Hgb F increased,
* Hgb A2 variable

PATHOGENESIS
Mutations causing thalassemia can affect any step of the pathway of globin-gene expression. The most common forma arise from mutations that derange spicing of the mRNA-precursor or prematurely terminate translation of the mRNA. More than 125 point mutations described, but 5-6 account for >90% of cases. A number of different mutations can cause reduced or absent β globin synthesis. Two major groups of mutations can be distinguished:
β-tal0: silenced gene
β-tal+: reduced synthesis (liable to patients with a milder phenotype, β-Thalassemia Intermedia)
Alleles associated with milder synthetic defect and co-inheritance of α-Thalassemia Trait reduce clinical severity by reducing accumulation of excess α globin.

