Martina Sanlorenzo Stefania Benetti
DEFINITION
Pemphigus is an autoimmune disease characterized by intraepidermal blisters and extensive erosions on apparently healthy skin and mucous membranes.The disease is characterized by the presence of autoantibodies directed against intercellular adhesion molecules desmoglein-1 and desmoglein-3 in the epidermis. They are Ca-dependent cadherins , involved in adhesion and cell signaling between epidermal cells.

Acantholysis result from either direct inhibition of function of the desmogleins by autoantibody binding or from autoantibody-induced cell signaling that results in down-regulation of cell-cell adhesion and formation of blisters. These autoantibodies are present in both serum and skin during active disease. Any area of stratified squamous epithelium may be affected, including mucosal surfaces.
EPIDEMIOLOGY
Pemphigus vulgaris is a rare (1/1000000) disease. It is found mainly in people of Ashkenazi Jewish descent and the age of onset if 60 years.
SYMPTOMS AND SIGNS
Mucous membranes typically are affected first in PV. Mucosal lesions may precede cutaneous lesions by months. Patients with mucosal lesions may present to dentists, oral surgeons, or gynecologists.
- Mucous membranes
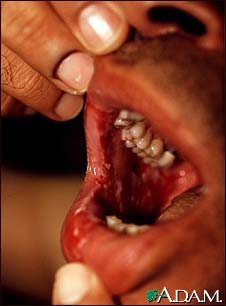
- Intact bullae are rare in the mouth. More commonly, patients have ill-defined, irregularly shaped, gingival, buccal or palatine erosions, which are painful and slow to heal. The erosions extend peripherally with shedding of the epithelium.
- The mucous membranes most often affected are those of the oral cavity, which is involved in almost all patients with PV and sometimes is the only area involved. Erosions may be seen on any part of the oral cavity. Erosions can be scattered and often extensive. Erosions may spread to involve the larynx with subsequent hoarseness. The patient often is unable to eat or drink adequately because the erosions are so uncomfortable.
- Other mucosal surfaces may be involved, including the conjunctiva, esophagus, labia, vagina, cervix, penis, urethra, and anus.
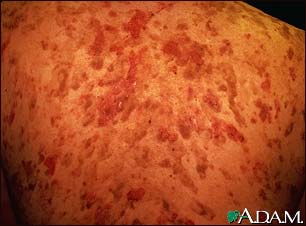
- Skin: The primary lesion of PV is a flaccid blister filled with clear fluid that arises on normal skin or on an erythematous base. The blisters are fragile; therefore, intact blisters may be sparse. The contents soon become turbid, or the blisters rupture producing painful erosions, which is the most common skin presentation. Erosions often are large because of their tendency to extend peripherally with the shedding of the epithelium.
- Vegetating PV: Ordinary PV erosions may develop vegetation. Lesions in skin folds readily form vegetating granulations. In some patients, erosions tend to develop excessive granulation tissue and crusting, and these patients display more vegetating lesions. This type of lesion tends to occur more frequently in intertriginous areas and on the scalp or face. The vegetating type of response can be more resistant to therapy and can remain in one place for long periods of time.
- Nails : Acute paronychia, subungual hematomas, and nail dystrophies have been reported with PV.
- Nikolsky sign : In patients with active blistering, firm sliding pressure with a finger separates normal-appearing epidermis, producing an erosion. This sign is not specific for PV and is found in other active blistering diseases.
- Asboe-Hansen sign: Lateral pressure on the edge of a blister may spread the blister into clinically unaffected skin.
DIAGNOSIS
Skin biopsy's usually show intraepidermal bulla, eosinophiul infiltrate and acantholysis, which refers to the separation of epidermal cells. Direct and indirect immunofluorescence, the presence of immunoglobulin G and complement C3 within the affected areas, and antibodies directed against desmoglein 3, a cellular adhesion molecule all aid in diagnosis. Prognosis is usually done by following antibody levels.

TREATMENT
Severe cases of pemphigus are treated similarly to severe burns. Treatment may require hospitalization, including care in a burn unit or intensive care unit. Treatment is aimed at reducing symptoms and preventing complications.
- Treatment may involve:
- Fluids, proteins, and electrolytes given through a vein (IV)
- IV feedings if there are severe mouth ulcers
- Anesthetic (numbing) mouth lozenges to reduce mouth ulcer pain
- Antibiotics and antifungal medications to control or prevent infections
Body-wide (systemic) therapy is needed to control pemphigus and should be started as early as possible. Systemic treatment includes corticosteroids, medications containing gold, an anti-inflammatory drug called dapsone, and medications that suppress the immune system (such as azathioprine, methotrexate, cyclosporin, cyclophosphamide, or mycophenolate mofetil). However, side effects from systemic therapy are a major complication.
Some antibiotics are also effective, particularly minocycline and doxycycline.
The combination of rituximab and intravenous immune globulin is effective in patients with refractory pemphigus vulgaris.
Plasmapheresis is a process whereby antibody-containing plasma is removed from the blood and replaced with intravenous fluids or donated plasma. Plasmapheresis may be used in addition to the systemic medications to reduce the amount of antibodies in the bloodstream.
Localized treatment of ulcers and blisters may include soothing or drying lotions, wet dressings, or similar measures.