FORMATION OF HARD TISSUES OF THE TOOTH
It includes the processes with which ends the late phase of bell stage: the amelogenesis, dentinogenesis and cementogenesis.
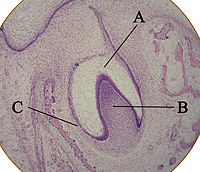
Dentinogenesis. The dentin genesis always occurs before amelogenesis. Odontoblasts differentiate from cells of the dental papilla. They begin secreting an organic matrix (pre-dentin) around the area directly adjacent to the inner enamenl epithelium. The organic matrix contains collagen fibers. The odontoblast start to move toward the centre of the tooth, forming an extension, the odontoblastic process, which is contained in the dentin tubules and causes the secretion of hydroxyapatite crystals. The first dentin formed is mantle dentin, then primary dentin. Dentin formation of the first crystals is correlated with the presence of matrix vesicles. Calcium phosphate ions are transported within vesicles and mineralization begins with the formation of hydroxy-apatite crystals whose growth, with the formation of other crystals, causes the rupture of vesicles and the deposition of crystals in the matrix. Whereas mantle dentin forms the pre-existing ground substance of the dental papilla, primary dentin forms through a different process. Odontoblasts increase in size, eliminating the availability of any extracellular resources to contribute to an organic matrix for mineralization. Secondary dentin is formed faster along section closer to tooth crown and it occurs throughout the life as tertiary dentin which takes place for reparative processes.
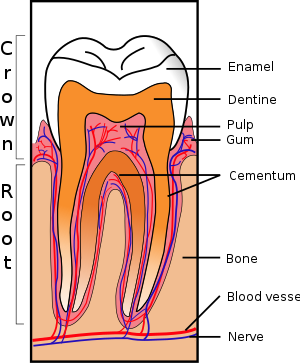
Amelogenesis. The deposition of the organic matrix of enamel begins after the first deposition pre-dentin. Unlike other mineralized tissues, enamel can be seen in two stages: secretory and maturation stage.
- In the secretory stage, the ameloblasts release enamel proteins that contribute to the enamel matrix (a 100 nanometers layer) which is partly mineralized by alkaline phosphatase in hydroxyapatite crystals: the formed enamel is not prismatic. Shortly after his deposition in the secretory pole of ameloblast originates a wedge-shaped cytoplasmic extension, the process of Tomes. Here, deposition of organic matrix and its partial digestion occur, so ameloblasts drawing back towards external epithelium and deposit an organic matrix rich in amelogenins reaching a final thickness equal to the crown of the tooth and provide for mineralization of hydroxyapatite crystals. The amelogenins are in a state of "gel", but have a typical thixotropy and therefore a strong ability to transform the status of "sol" for pressure stimulus and returning to the initial status at the end of the stimulus. The pressure that is created during the growth of crystals may cause a matrix change in the state of sol and then a draw back to the enamel in formation. The replacement of amelogenins with enameline and their degradation may still involve a process of secretion by ameloblast specific proteases or other enzymes.
- Maturation phase: This phase is characterized by a complete mineralization of the tissue deposited. The hydroxyapatite crystals are enhanced, reaching the final diameter of 50-100 nm, but a reduction in protein and water present take place. Before the last layer of organic matrix deposition, the ameloblasts become shorter, while the process of Tomes disappears in order to be replaced by a plasma membrane with a smooth surface. The "maturation" of the glaze covers a period from the deposition of the organic matrix to complete eruption of the tooth in dental. Ca2+ ions are placed in front of mineralization by vesicles of ameloblasts during the secretory phase, while the spread between ameloblast during ripening.
Cementogenesis. It occurs late in the tooth development and the cell involved are cementoblasts which form acellular first and the cellular cementum. The cementoblasts differentiate from follicular cells and reach the root after Hertwig’s Epithelial Root Sheath has deteriorated. They secret collagen fibrils. When mineralization begins, cementoblasts move away from cementum. Cellular cementum develops when teeth are completely formed in oral cavity: the cementoblasts become trapped in the cementum they produce. In premolar and molar this kind of cementumis localized next to apex and in interradicular areas between multiple roots.
Tooth Development
 Amelogenesis imperfecta phenotype-genotype correlations with two amelogenin gene mutations
Amelogenesis imperfecta phenotype-genotype correlations with two amelogenin gene mutations
 Bone morphogenetic protein-7 (osteogenic protein-1, OP-1) and tooth development
Bone morphogenetic protein-7 (osteogenic protein-1, OP-1) and tooth development
 IGFs increase enamel formation by inducing expression of enamel mineralizing specific genes
IGFs increase enamel formation by inducing expression of enamel mineralizing specific genes
Tetracycline are an antibiotic medicine consisting of four condensed rings like tetracene, partly hydrogenated with hydroxyl, ketone, a dimethylamino and a amide groups.
Hydroxyl groups have an alfa direction and may compose chelate which interact with ribosomal 30s subunit (if bounded to Mg), or influence collagen biosynthesis by inhibiting pocollagen hydroxylase (if bounded to Fe).

FEATURES
• Not much soluble
• Anphoteric
• In acid pH, it becomes an epimer and deteriorates into an inactive molecule: anhydrotetracycline
• In basic pH, it becomes isotetracycline by ring broke and forming a heterocycle.


SIDE EFFECTS
• Tetracycline should be used with caution in case of patients with liver impairment and they may cause renal failure (except doxycycline and minocycline)
• They may increase muscle weakness in myasthenia gravis and exacerbate LES
• Like many antibiotics, they decrease the effectiveness of birth control pills.
• The breakdown products of tetracycline are toxic and can cause Fanconi syndrome a potentially fatal disease affecting proximal tubular function in the nephrons of the kidney.
• They may cause stomach or bowel upsets, and rarely allergic reactions. Very rarely severe headache and vision problems may be signs of dangerous secondary intracranial hypertension also known as Pseudotumor cerebri.
• Some patients taking tetracycline require medical supervision because they can cause steatosis and hepatotoxicity.
• In case of long term therapy, they may cause bone deformation, due to their capability to chelate Ca, and intestinal diseases, because of suppression of intestinal micro flora (favoring Candida or Pseudomonas).
SIDE EFFFECT ON TOOTH DEVELOPMENT

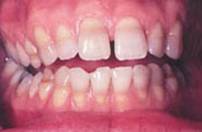
• Tetracycline cause teeth discolouration. They interact in two different way:
1. A therapy based on tetracycline during the devolpment of tooth, particularly in dentinogenesis and amelogenesis, causes a distruction of ameloblasts, a dischroma and dentin exposure. This event is irreversible, causing an aesthetic damage and erosion of discovered dentin; so the odontoiatric aim is preserving the dental element as long as possible searching a good compromise between aesthetics and functionality.
2. dentinogenesis. They promote the mineralization substituting collagen fibers and they participate to the formation of Ca salts with particular fluorescence. It occurs:
- in tooth development (primary dentin)
- all the life (secondary dentine)
- for external insults (tertiary dentin).
That's why, a somministration of tetracycline may induce a deposition of Ca salts bounded to tetracycline molecules all life long.
3. amelogenesis. Tetracycline bind to Ca in the ameloblastic’s vesicles during the secretive phase; because of that they confer the typical browning in the teeth.
 Quantitative analysis of KTP laser photodynamic bleaching of tetracycline-discolored teeth
Quantitative analysis of KTP laser photodynamic bleaching of tetracycline-discolored teeth
 Treating tetracycline staining in the adult dentition: a case report
Treating tetracycline staining in the adult dentition: a case report
di Camisassa Davide e Petrolo Francesco