Mycosis
Mycosis are infections caused by microscopic fungus. Depending on their morphology, their are divided in:
- yeast;
- dimorphic mycete;
- mold
Some of thiese microorganisms are commonly being on the skin or in the organism without leading to any damage; these lead to mycosis:
- cutaneous or mucocutaneous;
- deep;
The first, less serious and more frequent, strikes skin, skin folds, toes, scalp, nails, mouth and genitalia. This includes candidiasi (white mouth, balanitis) and dermatophytosis (tinea, athlete foot,herpes). Sometimes it occurs if extensive antibiotics; its appearance is favourite by poor hygiene.
The second is, contrarily, a more serious form and appears only in immunosuppressed individuals (patients undergoing organ transplantation, treated with chemioterapic, immunosuppressive and corticosteroids, AIDS patients and heroin addicts). Candidias infections can take, in fact, the form of a septicemia with extension to endocardium, lungs, meninges and kidney.
Candida Albicans
The most frequent between human pathogen Candida species. This yeast occurs naturally in mouth, in gastrointestinal tract and genitalia. It usually remains confined, but, in anomalous conditions, it can be located elsewhere.
It can release about 80 different type of toxins, which can be released into circulation. After a silent period of growth, C. can evolve in fungus. It is a microorganism with a strong adaptability to environment, which it reproduce in and it can choose to differentiate into 2 forms emitting root offshoots, Rizoides.
Fungus can penetrate actively in epithelium with esoenzymes help, where cell membrane enzymes lyse host cell. It comes in the form of spores and hyphoes. The second form is regulated as one capable to invide tissues colonized and injury. This injuries are the result of the complex interaction between fungus pathogenicity, host immunitary state and organism microenvironment. The mechanisms underlying the pathogenicity are adherence to ephitelial cell, the transformation in hyohoes, cheratinolytic enzymes production (protease), virulent phenotypes selection.
Candidiasis
Candidiasis, also called Monilliasis, is a very common fungal infection.Oral candidiasis is often observed as a local opportunistic infection and is clinically divided into three types: acute forms, chronic forms, and Candida-associated lesions. Additionally, it is divided into
- Systemic candidias;
- Localised candidias.
The first takes place in immunocompromised individuals; it can involve the esophagus and become systemic. In severe cases C. multiplies in an abnormal manner and, through the intestine, can reach the blood where free its toxins causing Candidemia.
The second takes place in patients without impairment of immune functions and moist part of body, for ex:
- Oral cavity (white thrush)
- Vagina (vulvovaginitis by C.)
- Penis (male genitalia in general)
In cases of sistemic candidias, the disease results in bloating, slow digestion, intestinal constipation and diarrhea. Consequently there is poor absorption of nutrients.
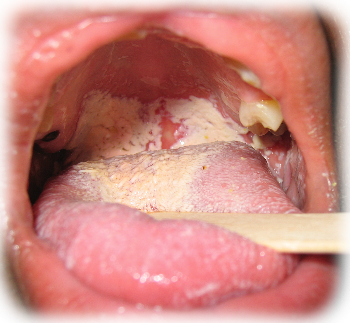
Oral Candidiasis

Strictly speaking, thrush is only a temporary candida infection in the oral cavity of babies. But we have, for this purpose, expanded the term to include candida infections occurring in the mouth and throat of adults, also known as candidiasis or moniliasis.This pathology is a fungal infection of mucosas, often this is in conjuinction with a health general compromise. In many case is caused by Candida Albicans, also called Monilia, or by Aspergillus and appear mainly in children and elderly diabetics, in wearers of dentures and in Aids patients. It can be spread to nearby organs or by blood, causing mycotic pneumonia, mycotic encephalitis, mycotic sepsis.
Symptoms
Initially, you may not have noticeable oral thrush symptoms. Signs and symptoms may develop suddenly, but they may persist for a long time and can include:
- Creamy, white lesions on your tongue, inner cheeks and sometimes on the roof of your mouth, gums and tonsils
- Lesions with a cottage cheese-like appearance
- Pain
- Slight bleeding if the lesions are rubbed or scraped
- Cracking at the corners of your mouth
- A cottony feeling in your mouth
- Loss of taste
Candida overgrowth in the oral cavity may disseminate to distant organs. Therefore, in order to avoid the sequelae of systemic candidiasis, oral candidias can be rapidly controlled.
Infants and breast-feeding mothers
In addition to the distinctive white mouth lesions, infants may have trouble feeding or be fussy and irritable. They can also pass the infection to their mothers during breast-feeding. The infection may then pass back and forth between mother's breasts and baby's mouth. Women whose breasts are infected with Candida may experience the following signs and symptoms:
- Unusually red, sensitive or itchy nipples,
- Shiny or flaky skin on the areola,
- Unusual pain during nursing or painful nipples between feedings,
- Stabbing pains deep within the breast.
Causes
C. lives as a guest in all individuals and does not bacame dangerous until:
- Immune system is functionally efficient
- Intestinal and oral ph are optimal
- There is a stable populatin of bacterial flora in colon
Candisias can became dangerous when this conditions lack, so it turns his friendly form of yeast into fungus, and begin to invade body creating problems. We talk about CHRONIC CANDIDIAS SYNDROME or CCS. Other proliferative conditions are:
- Use of venture
- Use of antibiotics, corticosteroids, anti-inflammatory, immusosuppressive therapy
- Spontaneous hormonal changes
- Smoking and alcohol
- Abuse of sugar and milk derivated
- Lack of rest
- Lack of exercise
- Prolonged illnesses that stress the body
- Presence of toxic metals (mercury) in body
- Leucomas
- Lack of vit.A (this is involved in the protection of patients suffering from leukoplakia)
Lack of vitamine A is involved in development of some oral mucose lesion as angular cheilitis.
It seems that Candida Albicans is probably responsible of some leukoplakias called
candidiasis leukoplakia.
Retinoic acid, derived from vit. A, is used for the treatment of disseminate candidiasis which may occur in case of promyelocitic leukemia refractory to chemotherapy.
Candidias can develop also in cases of pre-existing skin disorders or of mucosa because of external factors, hot, detergents, acids..). Oral C., specifically, is caused by predisposing factors like:
- Diabetes
- Prothesis
- Antibiotics therapy
- Antineoplastic therapy
- Invale or sistemic corticosteroids therapy
- HIV
Therapy
In patients with light oral candidiasis not associated to state of immunodeficiency, is sufficient a treatment with local antifungals.
antifungal
Polyene antifungal
These drugs include amphotericin B and nystatin, first choise. In oral, orofaringeal infections are used like topic applications. Amphotercin B is an active drug against yeasts and fungi. When given parenterally is toxic and causes many collateral effects.
Amfotericina B
amfotericina B
Imidazole antifungal
Imidazolo antifungals include local treatments like clotrimazole, econazole, ketoconazole, sulconazole, tioconazole.
Miconazole can be used topically in the oral infections. It can be absorbed and this can cause negative effects.
Triazole antifungals
Il fluconazole is well absorbed when given orally.
fluconazole
L’itraconazolo is associated with an hepatic damage. itraconazole