TOURETTE SYNDROME
DEFINITION AND SYMPTOMS
Tourette syndrome is a complex neurological disorder that usually becomes evident between 4 and 18 years of age. It is characterized by chronic motor and phonic tics, often with a variety of behavioural comorbidities. Tics can be suppressed temporarily, and are preceded by a premonitory urge, that is an uncomfortable bodily sensation, such as an itch, a tingle or tension. Some with Tourette syndrome will describe a need to complete a tic in a certain way or a certain number of times in order to relieve the urge or decrease the sensation.
Patients with eye movement tics were younger at age of Tourette syndrome onset (7.1 ± 4 years) than those without (8.9 ± 6.8 years). Tic severity positively correlated to lifetime history of eye and/or eyelid/eyebrow movement tics. Most patients have several types of eye tics over time. Eye tics are therefore likely to be a core feature of Tourette syndrome and should be routinely evaluated in order to strengthen the clinician's confidence in diagnosing the syndrome.
In addition to eye blinking and eye movements, other tics include facial grimacing, shoulder shrugging, and head or shoulder jerking. Simple vocalizations might include repetitive throat-clearing, sniffing, or grunting sounds. Complex tics are distinct, coordinated patterns of movements involving several muscle groups. Complex motor tics might include facial grimacing combined with a head twist and a shoulder shrug. Other complex motor tics include sniffing or touching objects, hopping, jumping, bending, or twisting. Simple vocal tics may include throat-clearing, sniffing/snorting, grunting, or barking. More complex vocal tics include words or phrases. Perhaps the most dramatic and disabling tics include motor movements that result in self-harm such as punching oneself in the face or vocal tics including coprolalia (uttering socially inappropriate words such) or echolalia (repeating the words or phrases of others). However, coprolalia is only present in a small number (10 to 15 percent) of individuals with TS.
Tourette syndrome
Prevalence and phenomenology of eye tics in Gilles de la Tourette syndrome
COMORBIDITIES
Many patients with Tourette syndrome report additional neurobehavioral problems that often cause more impairment than the tics themselves. These include inattention, hyperactivity and impulsivity (attention deficit hyperactivity disorder or ADHD); problems with reading, writing and arithmetic; obsessive-compulsive symptoms such as intrusive thoughts or worries and repetitive behaviors. For example, worries about dirt and germs may be associated with repetitive hand-washing, and concerns about bad things happening may be associated with ritualistic behaviors such as counting, repeating, or ordering. People with Tourette syndrome have also reported problems with depression or anxiety disorders, as well as other difficulties with living, that may or may not be directly related to Tourette syndrome. In addition, although most individuals with Tourette syndrome experience a significant decline in motor and vocal tics in late adolescence and early adulthood, the associated neurobehavioral conditions may persist.
Tourette Syndrome Fact Sheet
DIAGNOSIS
Tourette’s may be diagnosed when a person exhibits both multiple motor and one or more vocal tics over the period of a year, with no more than three consecutive tic-free months. The onset must have occurred before the age of 18, and cannot be attributed to the "direct physiological effects of a substance or a general medical condition". There are no specific medical or screening tests that can be used in diagnosing Tourette's; it is frequently misdiagnosed or underdiagnosed, partly because of the wide expression of severity, ranging from mild (the majority of cases) or moderate, to severe (the rare, but more widely-recognized and publicized cases). The diagnosis is made based on observation of the individual's symptoms and family history. There is no requirement that other comorbid conditions be present, but if a physician believes that there may be another condition present that could explain tics, tests may be ordered as necessary to rule out that condition. An example of this is when diagnostic confusion between tics and seizure activity exists, which would call for an EEG, or if there are symptoms that indicate an MRI to rule out brain abnormalities. TSH levels can be measured to rule out hypothyroidism, which can be a cause of tics. In teenagers and adults presenting with a sudden onset of tics and other behavioral symptoms, a urine drug screen for cocaine and stimulants might be necessary. If a family history of liver disease is present, serum copper and ceruloplasmin levels can rule out Wilson's disease.
PATHOPHYSIOLOGY
The cause of Tourette syndrome is poorly understood. Although environmental factors are proposed to have a role, genetic factors are thought to be the primary contributors to the pathogenesis of this disorder. However, identification of the causative gene mutations or risk alleles has proved to be difficult. Tics are believed to result from dysfunction in cortical and subcortical regions, the thalamus, basal ganglia and frontal cortex. Greater putamen dopamine release was seen in adults with Tourette's syndrome than in comparison subjects after a pharmacologic challenge with amphetamine. These results suggest that the underlying pathobiology in Tourette's syndrome is a phasic dysfunction of dopamine transmission. Recent studies provide evidence implicating metabolic abnormalities of dopamine (DA) and serotonin (5-HT) of the basal ganglia both in patients and animal models. It is also well known that dopamine and serotonin transporters (DAT and SERT) are monoamine neurotransmitter transporters, which participate in the metabolism of DA and 5-HT, respectively. Lower expression in DAT, concomitant with higher expression in SERT could participate in the pathophysiology of Tourette. The DA concentration in striatum homogenate was higher in the Tuorette model group than in the control group, but 5-HT concentration in striatum was found to be lower in the Tourette model group compared to the control group.
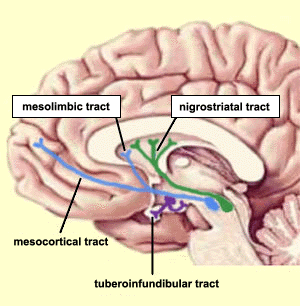
Dopaminergic pathways
The genetics of Tourette syndrome
Elevated intrasynaptic dopamine release in Tourette's syndrome
Abnormal expression of dopamine and serotonin transporters associated with the pathophysiologic mechanism of Tourette syndrome
TREATMENT
The disorder can lead to serious impairments of both quality of life and psychosocial functioning, particularly for those individuals displaying complex tics. In such patients, drug treatment is recommended. The pathophysiology of Tourette syndrome is thought to involve a dysfunction of basal ganglia-related circuits and hyperactive dopaminergic innervations. Congruently, dopamine receptor antagonism of neuroleptics appears to be the most efficacious approach for pharmacological intervention (for example, haloperidol, pimozide, risperidone, ziprasidone and fluphenazine). The antihypertensive agents clonidine and guanfacine are also used to treat tics; studies show variable efficacy, but a lower side effect profile than the neuroleptics.
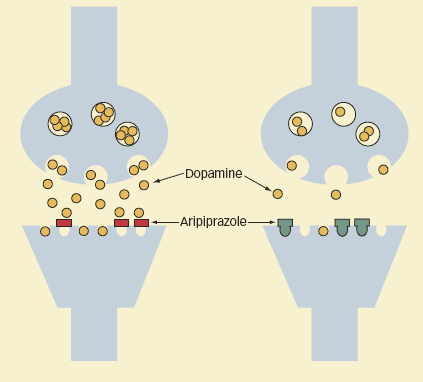
Dopamine receptors
Not everyone with Tourette's wants treatment or a "cure", especially if that means they may "lose" something else in the process. Children with "Tourette-only" (Tourette's in the absence of comorbid conditions) are unusually gifted: one study found that children with Tourette-only are faster than the average for their age group on timed tests of motor coordination.
Notable individuals with Tourette syndrome are found in all walks of life, including musicians, athletes, media figures, teachers, physicians and authors.The best-known example of a person who may have used obsessive–compulsive traits to advantage is Samuel Johnson, the 18th-century English man of letters, who likely had Tourette syndrome as evidenced by the writings of James Boswell. Johnson wrote A Dictionary of the English Language in 1747, and was a prolific writer, poet, and critic.
Sociological and cultural aspects of Tourette syndrome