Allergic conjunctivitis
Definition
Allergic conjunctivitis is inflammation of the conjunctiva (the membrane covering the white part of the eye) due to allergy.
Allergic conjunctivitis is common, especially during the allergy season. Allergic conjunctivitis affects up to 40% of the general population and is a common clinical problem for ophthalmic and allergic practices. Allergic Conjunctivitis has a huge market potential of >1 billion USD.
Useful links:
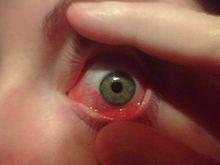
The cause of allergic conjunctivitis is an allergic reaction of the body's immune system to anallergen. Allergic conjunctivitis is common in people who have other signs of allergic disease such as hay fever, asthma and eczema.
Among the most common allergens that cause conjunctivitis are:
* Pollen from trees, grass and ragween
* Animal skin and secretions such as saliva
* Perfumes
* Cosmetics
* Skin medicines
* Air pollution
* Smoke
* Dust mites
* Eye drops
Allergic conjunctivitis subtypes
Allergic conjunctivitis may be divided into 5 major subcategories.
- Seasonal allergic conjunctivitis (SAC) Caused by number of allergens. Presents as a triad of itching,redness and swelling.
- Perennial allergic conjunctivitis (PAC) Caused by airborne allergens. Symptoms are similar to those in SAC.
- Vernal keratoconjunctivitis (VKC) Formation of large, raised, cobblestone papillae of the upper tarsal conjunctiva.
- Giant papillary conjunctivitis (GPC) Chronic inflammatory disorder of the upper tarsal conjunctiva constitute the remaining subtypes of allergic conjunctivitis.
- Atopic keratoconjunctivitis (AKC) is a bilateral inflammation of conjunctiva and eyelids, which has a strong association with atopic dermatitis.
Pathophysiology
The eye represents an ideal and frequent site for the allergic reactions. The term ‘ allergic conjunctivitis ’ refers to a collection of disorders that affect the lid, conjunctiva and/or cornea. Even though the diagnosis is essentially clinical, local tests such as cytology, conjunctival provocation and tear mediator
analysis can be performed. The immunoglobulin E (IgE)mediated mechanism does not explain completely the severity and the clinical course of chronic allergic ocular diseases such as vernal (VKC) and atopic keratoconjunctivitis (AKC), which are probably also related to T cell-mediated responses, massive eosinophil attraction and activation and non-specific hypersensitivity. An altered balance between T helper type 1 (Th1) and Th2 cells and between Th1- and Th2-types of cytokines is thought to be responsible of the development of ocular allergic disorders. New findings suggest that a wide range of cytokines, chemokines, proteases and growth factors are involved by complex interwoven interactions rather than distinct and parallel pathways. In addition, several non-specific enzymatic systems may be activated during acute and chronic allergic inflammation, thus contributing to the complex pathogenesis of the disease. Current drug treatment for ocular allergy targets the key mechanisms involved in the development of clinical disease: mast cells with mast cell stabilizers, histamine with histamine receptor antagonists and inflammation with corticosteroids, severe inflammation with immunomodulators. None of these agents lacks side effects and none abolishes signs and symptoms completely. New therapeutic strategies are still needed to respond to the complex pathogenesis of severe forms of ocular allergy such as VKC and AKC.

Mast cell mediated allergic response mechanisms.


A detailed history may reveal recent exposure to individuals who have conjunctivitis or upper respiratory tract infection within the family, school, or workplace. Such a history may help confirm an adenovirus infection in an endemic area. Knowledge of the patient's sexual activities and any associated discharge may suggest chlamydial disease or Neisseria infection. Frequently, the patient does not mention the use of over-the-counter topical medications such as vasoconstrictors or artificial tears, cosmetics, or contact lens wear. Direct questioning often reveals the use of these products or other topical and systemic medications, which are capable of producing inflammation that can mimic seasonal allergic conjunctivitis (SAC) or perennial allergic conjunctivitis (PAC). Knowledge of any systemic disease such as rheumatoid arthritis or other collagen vascular diseases raises the clinician's suspicion for keratoconjunctivitis sicca, although a patient referred for irritated eyes who has thyroid dysfunction suggests superior limbic keratoconjunctivitis.
The offending allergens vary from one location to another, but the symptoms appear to be similar throughout the world. Often, symptoms are not severe enough to precipitate a visit to the allergist or the ophthalmologist. Among patients who seek help, some may not require treatment and others may simply be able to avoid the allergens responsible for their disease.
Symptoms usually consist of low-grade ocular and periocular itching (pruritus), tearing (epiphora), burning, stinging, photophobia, and watery discharge. Redness and itching seem to be the most consistent symptoms. Although symptoms persist throughout the allergy season, they are subject to exacerbations and remission, depending on the weather and the patient's activities. Symptoms are generally worse when the weather is warm and dry; cooler temperatures and rain tend to alleviate symptoms. Although itching is generally mild, occasionally it can be severe, and rarely patients may be incapacitated by their symptoms. Many of the symptoms of ocular allergy are nonspecific, such as tearing, irritation, stinging, burning, and photophobia.
The symptom of itching is strikingly characteristic of allergic conjunctivitis. It is often said that ocular itching implies allergy until proven otherwise. Furthermore, ocular itching is rare in other conditions, although it is not unknown. Patients who have blepharitis, dry eye, and other types of conjunctivitis may experience itching. It is worthwhile to pinpoint the location of itching. For example, patients who complain of ocular itching may be presumed to be describing conjunctival itching; however, some patients who have ocular itching describe symptoms related to the skin of their eyelids. Careful questioning can distinguish itching of the conjunctiva from itching of the eyelid skin. Although the former is usually associated with allergic rhinoconjunctivitis, which affects the conjunctiva, the latter may indicate contact allergy, which affects the skin and the conjunctiva. The discharge is usually watery and may be described as tearing. Sometimes there is a scan mucus component. The discharge may range from serous (watery) to mucopurulent and grossly purulent. A stringy or ropy discharge is characteristic of allergy. In severe forms of allergic conjunctivitis, such as vernal conjunctivitis, tenacious strands of mucus can be removed from the eye by the patient or the doctor. Environmental allergens are ubiquitous and nonselective, most commonly affecting both eyes at the same time. Conjunctival injection is commonly associated with discomfort, and when the patient complains of ocular pain, the physician must search for other causes.
In allergic patients, it is unusual to have conjunctival symptoms without nasal symptoms . The nasal mucosa is expected to react in the same fashion as the conjunctival mucosa; however, at times the physician encounters allergic patients whose symptoms appear to be ocular. These patients may indicate that they do not have systemic allergies because they have not experienced typical allergic rhinitis. It is not known why the conjunctiva should be the main target in certain patients who have allergies. There may be emotional or psychologic factors that make ocular symptoms more disturbing than nasal symptoms. Often, when patients deny nasal or respiratory symptoms, careful questioning can sometimes elicit such symptoms, even though they may be mild.
Diagnosis
The eye should be carefully examined for evidence of eyelid involvement (ie, blepharitis, dermatitis, swelling, discoloration, ptosis, blepharospasm), conjunctival involvement (ie, chemosis), hyperemia, palpebral and bulbar papillae, cicatrization, and presence of increased or abnormal-appearing secretions. In addition, a funduscopic examination should be performed for uveitis associated with autoimmune disorders and chronic steroid use.
Scraping the conjunctival surface to look for eosinophils is a helpful diagnostic test. The procedure is done by placing a drop of topical anesthetic such as tetracaine hydrochloride 0.5% in the lower conjunctival sac. The anesthetic takes effect within 10 seconds. Using a platinum spatula, the inner surface of the lower lid is gently scraped several times. The material is then spread on a microscope slide. The slide is stained with Hansel stain, Giemsa stain, or another common reagent. Slides are examined for the presence of eosinophils or eosinophil granules. Eosinophils are not ordinarily found in the conjunctival scrapings from nonallergic individuals. The presence of even one eosinophil or eosinophil granule is considerable evidence in favor of a diagnosis of allergic conjunctivitis . The absence of eosinophils should not rule out a diagnosis of allergy. Eosinophils are often present in the deeper layers of the conjunctiva and may be absent or undetectable in the upper layers. The frequency of eosinophils in the conjunctival scrapings from patients who have allergic conjunctivitis may vary from 20% to 80% depending on the patient population, the chronicity of the allergic condition, and the persistence of the examiner . Corneal infiltrates may occasionally be seen in severe allergic patients and tend to be nummular, subepithelial, and peripheral.
Conjunctival provocation tests (CPTs), which consist of instilling an offending pollen into the conjunctival sac, also produce the typical symptoms of hay fever conjunctivitis and were the original method for evaluating allergic responses. Ocular challenge is used as a pharmacologic model for the evaluation of new antiallergic medications and immunotherapy . The positivity of the challenge may be assessed by a sign and symptom scoring system that includes subjective and objective signs such as conjunctival erythema, chemosis, tearing, and pruritus. CPTs have also been shown to have a relatively good reproducibility in both eyes . A CPT of ocular mast cells by way of opioid receptors has shown that 80% of normal patients reflect mast cell activation by detection of the release of histamine (7 versus 18 nm/L) and prostaglandin D2 (0 versus 273 ng/L). The release of these mediators can be blocked by pretreating patients with cromolyn. In assessing the potential usefulness of CPTs as a diagnostic tool, it was found that CPTs directly correlated to the radioallergosorbent test (RAST) in 71% (n = 130/183) of allergic patients. Of the 29% of uncorrelated cases, 23% (43/183) were positive by RAST but not by CPT, whereas 6% (10/183) were positive by CPT but not by RAST. This finding suggests that there may be local sensitization of the target organ without evidence for systemic sensitization to the same antigen that clinically may reflect allergens causing ocular symptoms without any evidence of pulmonary or nasal allergic symptoms.
For more Examination
Treatment
The best treatment is avoiding exposure to the cause or allergen. Unfortunately, this is not often practical. Discomfort can be relieved by applying cool compresses to the eyes or taking antihistamines by mouth (many of these are available over the counter).
If home-care measures do not help, treatment by the health care provider may be necessary.
Allergic conjunctivitis can be treated with a variety of drugs. These include topical antihistamines, mast cell stabilizers, nonsteroidal anti-inflammatory drugs (NSAIDs), and corticosteroids. As always, care must be taken when using topical corticosteroids; pulsed regimen is recommended to minimize adverse reactions.
Antihistamine, Ophthalmic
These agents act by competitive inhibition of histamine at the H1 receptor. They block the effects of endogenously released histamine.
Emedastine difumarate (Emadine)
This agent is a relatively selective H-receptor antagonist for topical administration.
Levocabastine
Levocabastine is a selective histamine H1 receptor antagonist.
Epinastine (Elestat)
A direct histamine-1 receptor antagonist, epinastine does not penetrate the blood-brain barrier and therefore should not induce adverse CNS effects. It is indicated for symptoms due to allergic conjunctivitis.
Azelastine ophthalmic (Optivar)
Azelastine competes with H1-receptor sites on effector cells and inhibits release of histamine and other mediators involved in allergic response.
Bepotastine besilate ophthalmic solution (Bepreve)
Bepotastine besilate is a topically active antihistamine that directly antagonizes H1-receptors and inhibits release of histamine from mast cells. It is indicated for itching associated with allergic conjunctivitis.
Alcaftadine ophthalmic (Lastacaft)
An H1-receptor antagonist indicated for prevention of itching associated with allergic conjunctivitis, alcaftadine inhibits histamine release from mast cells, decreases chemotaxis, and inhibits eosinophil activation.
Mast Cell Stabilizers
Mast cell stabilizers inhibit the degeneration of sensitized mast cells when exposed to specific antigens by inhibiting the release of mediators from the mast cells. These agents block calcium ions from entering the mast cell. Olopatadine is a relatively selective H1 receptor antagonist and inhibitor of histamine release from mast cells.
Lodoxamide tromethamine (Alomide)
Lodoxamide is a mast cell stabilizer. The active ingredient in this product is 1.78 mg lodoxamide tromethamine.
Olopatadine (Patanol, Pataday)
Olopatadine is a relatively selective H1 receptor antagonist and inhibitor of histamine release from mast cells.
Ketotifen (Zaditor, Alaway)
Ketotifen is an over-the-counter (OTC) antihistamine eye drop. It is a noncompetitive H1-receptor antagonist and mast cell stabilizer. This agent inhibits release of mediators from cells involved in hypersensitivity reactions.
Nedocromil ophthalmic (Alocril)
Nedocromil interferes with mast cell degranulation, specifically with release of leukotrienes and platelet activating factor.
Corticosteroids
Corticosteroids have both anti-inflammatory (glucocorticoid) and salt retaining (mineralocorticoid) properties. Glucocorticoids have profound and varied metabolic effects. In addition, these agents modify the body's immune response to diverse stimuli.
Loteprednol etabonate (Lotemax, Alrex)
This agent decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing increased capillary permeability. It is a topical ester steroid eye drop that poses a decreased risk of glaucoma.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
The mechanism of action of NSAIDs is believed to be through inhibition of the cyclooxygenase enzyme that is essential in the biosynthesis of prostaglandins, which results in vasoconstriction, decrease in vascular permeability and leukocytosis, and a decrease on intraocular pressure.
Ketorolac tromethamine (Acular, Acuvail)
A member of the pyrrolo-pyrrole group of NSAIDs, ketorolac inhibits prostaglandin synthesis by decreasing activity of the enzyme cyclooxygenase, which results in decreased formation of prostaglandin precursors.
Immunotherapy
Immunotherapy is a mainstay in the systemic management of allergies. Traditionally, immunotherapy is delivered via subcutaneous injection. However, sublingual (oral) immunotherapy (SLIT) is gaining momentum among allergists. Numerous articles have analyzed the effects of SLIT on allergic conjunctivitis. Preliminary indications are that SLIT may have a moderate effect on the signs and symptoms of allergic conjunctivitis, but further analysis is necessary.turn, this results in reduced inflammation.

For more Treatment Guidelines from The Medical Letter®