Liquorice or licorice is the root of Glycyrrhiza glabra (tall shrub of the Leguminosae family) from which a sweet flavor can be extracted. Glycyrrhizin (or glycyrrhizic acid or glycyrrhizinic acid, GA) is the main sweet-tasting compound from liquorice root (it constitutes 1-9% of licorice).
Licorice was a prescriptive agent of Hippocrates in the treatment for asthma, dry cough, and other “pectoral diseases,” and was also thought to be effective in preventing thirst. In Chinese traditional medicine, licorice remains one of the oldest and most commonly prescribed herbs.
The name Glycyrrhiza comes from the Greek words “glykos,” meaning sweet and “rhiza,” meaning root. Glycyrrhizin is reputed to be 50 times sweeter than refined sugar.
Glycyrrhizin (shown below) is a saponin compound comprised of a triterpenoid aglycone, glycyrrhetic acid (glycyrrhetinic acid) conjugated to a disaccharide of glucuronic acid. As a tribasic acid, glycyrrhizin can form a variety of salts and occurs naturally in licorice root as the calcium and potassium salts.

FDA acceptable daily intake is thought to be 0.015–0.229mg glycyrrhizin/kg body weight/day. Licorice is a very popular sweetener found in many soft drinks, food products (such as toffee and candies) snacks, chewing-gum and herbal medicines. It'is also used by tobacco's companies as a flavouring agent. It's particulary well-accepted by smokers when they are in “no-smoking” areas. A review concluded that about 2% of the regular consumers have a daily intake of glycyrrhizinic acid of over 100 mg/day [Mars, 2000]
Metabolism
Although GA can be occasionally administered intravenously, the general population is mainly exposed to GA by its consumption in various products. Glycyrrhizin has a poor oral bioavailability. The lipophilic components of licorice extract were found to reduce the gastric emptying rate and absorption of glycyrrhizin. Interestingly, neither glycyrrhizin nor glycyrrhetic acid are detected in the plasma of germ-free rats fed with glycyrrhizin. This suggests a presystemic metabolic process involving the de-glucuronidation of glycyrrhizin by intestinal flora prior to the absorption of glycyrrhetic acid. Indeed, researchers have identified various intestinal bacterial strains, including Streptococcus and Eubacterium sp., with specialized beta-glucuronidase activity capable of glycyrrhizin hydrolysis. Interindividual differences in glycyrrhizin response, metabolism and kinetics are therefore influenced, at least in part, by the intestinal microflora profile. Neither glycyrrhizin nor glycyrrhetic acid accumulate in tissues. In the bloodstream both compounds bind extensively to human and rat serum albumin. glycyrrhetic acid undergoes enterohepatic circulation: Analysis of the collected bile revealed the presence of three products of glycyrrhetic acid, indicating the hepatic conjugation of glycyrrhetic acid prior to biliary excretion:
*18beta-glycyrrhetyl-30-glucuronide (D),
*18beta-glycyrrhetyl-3-O-glucuronide ©,
*18beta-glycyrrhetyl-3-O-sulfate (B)

Because of the enterohepatic recycling of glycyrrhetic acid (shown in the figure below) and the biliary storage process of glycyrrhetic acid metabolites in the gallbladder, plasma glycyrrhetic acid concentrations show several peaks following the oral administration of either glycyrrhizin glycyrrhetic acid or licorice. Plasma clearance was significantly decreased in patients with chronic hepatitis C and liver cirrhosis.

From:
Risk and safety assessment on the consumption of Licorice root (Glycyrrhiza sp.), its extract and powder as a food ingredient, with emphasis on the pharmacology and toxicology of glycyrrhizin, 2006
Physiologically based pharmacokinetic modeling of glycyrrhizic acid, a compound subject to presystemic metabolism and enterohepatic cycling, 2000
Side effects of eccessive liquorice consumption
Glycyrrhizate compounds can induce the Apparent Mineralcorticoid Excess Syndrome (AME)
Anti-inflammatory properties
Literature survey showed that triterpenoids, as glycyrrhiic acid and others (ursolic acid, oleanolic acid...) had revealed immunomodulatory and antitumor properties. Glycyrrhizic acid can inhibit nuclear factor kappa B (NF-κB) signaling (Kang et al., 2005; Cherng et al., 2006) by suppressing IκB kinase (IKK)-mediated activation of NF-κB. NF-κB plays a key role in regulating the immune response to infection controlling the transcription of the genes involved. Glycyrrhizic acid has also been shown to inhibit glutamate-induced cytotoxicity in primary neurons (Cherng et al., 2006). Excitotoxicity due to excessive glutamate release and impaired uptake occurs as part of the ischemic cascade and is associated with stroke and diseases like amyotrophic lateral sclerosis, autism, some forms of mental retardation, and Alzheimer's disease.

From:
Inhibition of tumor progression by naturally occurring terpenoids, 2011
Antiviral effects
Historical sources for the use of Glycyrrhiza species include ancient manuscripts from China, India and Greece. There have been performed a lot of trials with different viruses, but the common effect is to induce γ-interferon, a potent endogenous inhibitor of viral replication, an immunostimulator for NK cells and macrophages.
Abe et al. examined whether glycyrrhizin or glycyrrhetic acids induce the production of interferon. Mice were inoculated with glycyrrhizin i.p. serum was then collected and tested for in vitro anti-viral activity in cells infected with vesicular stomatitis virus. The antiviral substance was recognized to be γ-interferon. interferon induction by glycyrrhizin is dependent on T-cell function. Inhibition of a glycyrrhizin-induced anti-viral titer by the previous treatment of mice with hydrocortisone, trypan blue, or X-rays may imply that lymphocytes and macrophages are also required for the induction of interferon by glycyrrhizin. An interesting finding was that when splenic T cells from glycyrrhizin-treated mice were transferred to mice exposed to a lethal dose of influenza virus, all the recipients survived, while no survivor was seen in recipient mice inoculated with native T cells, or with splenic B cells and macrophages from glycyrrhizintreated mice. The administration of glycyrrhizin to infected mice in combination with anti-gamma interferon monoclonal antibody did not produce any antiviral effect.
Glycyrrhizin has some specific effects on various viruses:
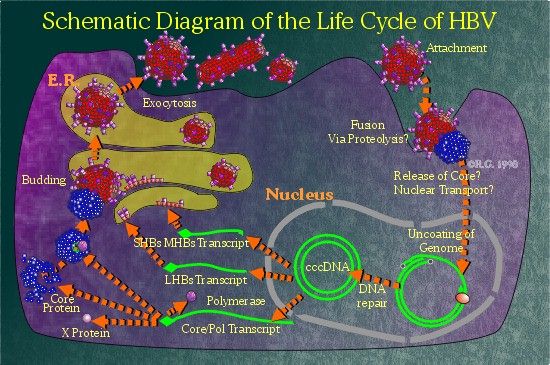
Hepatitis B and C Viruses:
The effect of a formulation (Stronger Neo-Minophagen C, SNMC) containing 40 mg glycyrrhizin, administered by injection were studied in randomized controlled trials involving patients with chronic viral hepatitis. Glycyrrhizin induced a significant reduction of serum alanine aminotransferase (ALT) and caused an improvement in liver histology, equivalent to those produced with interferon treatment. Following the use of SNMC, a retrospective study was conducted in Japan in order to evaluate the effect of glycyrrhizin on hepatocellular carcinoma development (Arase et al., 1997). Analysis disclosed that glycyrrhizin significantly decreased the hepatocarcinogenesis rate. In hepatitis B the virustatic effect could depend on inhibition of the intrahepatic transport and sialylation of the hepatitis B-virus (HBV) surface antigen (HBsAg) observed in vitro (Sato et al., 1996). Glycyrrhizin, suppressing the increase in phospholipase A2 activity and reducing membrane fluidity, inhibited the release of transaminases. It was found that 18-β-glycyrrhetic acid elicited a significant inhibitory action stronger than vitamin E is capable of inhibiting lipid peroxidation. Due to its properties as an immunomodulator, it reduces immuno-mediated cytotoxicity, which is the main cause of hepatocarcinogenesis.
Herpesviridae:
The antiviral effect of glycyrrhizin was evaluated in murine herpes encephalitis (Sekizawa et al., 2001). Intraperitoneal administration of glycyrrhizin increased the survival rate of the animals by about 2.5 times, and the viral replication in the brain was reduced to 45.6% of the control.
In studies demonstrating the inhibition of HSV-1 by glycyrrhizic acid in vitro a synergism of the inhibitory effect with the endogenous antiviral substance lactoferrin was found (Lampi et al., 2001). Glycyrrhizin demonstrated an additive effect with other conventional antiviral drugs such as acyclovir, and also with human beta-interferon.
An effect of glycyrrhizic acid was also reported against Epstein-Barr virus (EBV) The inhibition of EBV replication in vitro is dose-dependent. It has been suggested that the drug interferes with an early step of EBV replication, possibly penetration, without any effect on viral adsorption, or inactivation.
In Kaposi sarcoma-associated herpes virus (KSHV or HSV-8) it reduces the production of a viral latency protein and induces apoptosis in infected cells.
Influenza Virus:
Mice infected with influenza virus A2 (H2N2) were unable to survive 10 times the mean lethal dose (LD50) of virus. However, a complete survival was observed when these animals were treated with 10 mg glycyrrhizin/kg, i.p., on the day prior to, the day after, and on the fourth day after infection.
This same dosing regimen conferred 70% survival in mice infected with 50 times the viral LD50. The administration of glycyrrhizin to infected mice in combination with anti-gamma interferon monoclonal antibody did not produce any antiviral effect. Utsunomiya et al.
From:
Antiviral Effects of Glycyrrhiza species, 2008
Anti Vesicular Stomatitis Virus via increased synthesis of IFN gamma
Anti-cancer effect
GA has emerged as an attractive drug candidate for cancer therapy because of its apoptotic effect on tumor cells (Hibasami et al., 2005; Thirugnanam et al., 2008).
GA is been shown to inhibit angiogenesis. According to the recent reports, ROS play an important role in tumor angiogenesis; intracellular ROS production and mitochondrial ROS generation are decreased by treatment with GA. Glycyrrhiic acid may decrease the phosphorilation of ERK during the pathway that leads to angiogenesis (Kil-Jung Kim et al. 2012).

In tumor cell lines, multidrug resistance is often associated with an ATP-dependent decrease in cellular drug accumulation which is attributed to the overexpression of certain ATP-binding cassette (ABC) transporter proteins. ABC proteins that confer drug resistance include (but are not limited to) P-glycoprotein (gene symbol ABCB1), the multidrug resistance protein 1 (MRP1, gene symbol ABCC1) and others. (Leslie EM et al. 2005). Inhibitors of P-glycoprotein and MRP1 are useful not only to reverse or prevent acquired drug resistance, but also to sensitize drug-naïve untreated tumors to anticancer drugs. Therefore, MRP1 is also a promising target for the reversal of multidrug resistance and a better outcome of cancer chemotherapy. Glycyrrhetinic acid is a dual inhibitor of P-glycoprotein and MRP1. It is interesting that the inhibitory mechanisms of glycyrrhetinic acid might be different in the two ABC transporters. Glycyrrhetinic acid alone stimulated the basal ATPase activity of MRP1. In the presence of NEM-GS, an MRP1 substrate, the ATP hydrolysis by MRP1 was further stimulated by glycyrrhetinic acid. In contrast to the result of MRP1 ATPase activity, glycyrrhetinic acid alone had no effect on the ATPase activity of P-glycoprotein. However, glycyrrhetinic acid inhibited the verapamil-stimulated P-glycoprotein ATPase activity. These results suggest that glycyrrhetinic acid could be a substrate of MRP1, and competitively interact at drug-binding site of MRP1. In contrast, glycyrrhetinic acid is not a substrate of P-glycoprotein, but possibly interacts noncompetitively at ATP hydrolytic site of P-glycoprotein.
From:
Inhibition of P-glycoprotein and multidrug resistance protein 1 by dietary phytochemicals, 2008