MORGELLONS SYNDROME: REAL OR IMAGINARY?

DEFINITION
Morgellons syndrome (also known as Morgellons disease) takes its name from Mary Leitao (2002); even if it was recently named and acknowledged, the first reported cases of this strange disease date back to XVII century's France: at that time, the common feature linking the “supposed” patients were neurological symptoms (e.g. Epilepsy) and the presence of subcutaneous crawling parasite.
In fact, in this syndrome patients delusionally believe that they are infested with disease-causing agents described as things like insects, parasites, hairs or fibers, but in reality no such things are present. In 2006, Leitao's Morgellons Research Foundation started clinical studies which ended in 2012: results indicated that no organisms were found in Morgellons sufferers and this syndrome was associated to some kind of delusional infestation.
(Characterization and evolution of dermal filaments from patients with Morgellons disease, 2013)
EPIDEMIOLOGY
Based on recent statistic studies, Morgellons' sufferers are approximately 100'000, excluding eastern countries, aquatic and terrestrial animals; this statistic leads to the conclusion that the dark numbers of the infection can be about 10 million (if not more).
There are several ways of transmission, including:
1. contact with:
1.1 vegetal fibres
1.2 soil
1.3 animals (cats, dogs, horses, etc...)
1.4 skin (supposed)
2. genetic transmission
3. studies indicated that there is not sexual transmission
Furthermore, subjects with pre-existent Borrelia bacteria infections, causing Lyme disease, are more likely to present Morgellons syndrome.
(Morgellons disease: Analysis of a population with clinically confirmed microscopic subcutaneous fibers of unknown etiology, 2010)
(Morgellons epidemiology, 2010)
SYMPTOMS
The main problem with Morgellons syndrome is that it is apparently strictly related to Lyme disease: therefore, the “pure” symptoms can be divided in skin and internal ones.
For what concerns the skin, there are three stages:
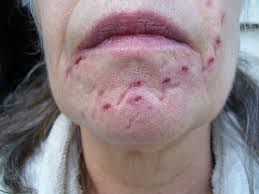
1. First the patient starts experiencing subcutaneous crawling sensations, especially around scalp, nose and mouth regions.
2. Subsequently, the sufferer claim to feel something biting, stinging and itching him.
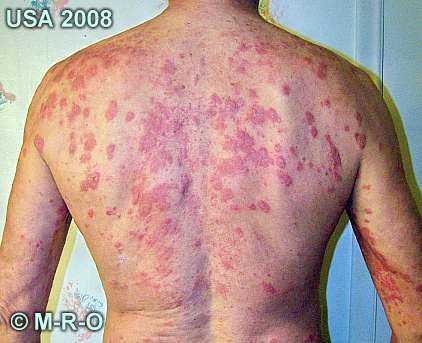
3. Finally, skin damage becomes more visible, as blisters, lesions pustules are visible; moreover, protruding fibres are visible.
Fibres, upon inspection, were found to be fluorescent. The fibers were visualized in scintillation vials with a Innotech detector, showing fluorescence with both a Hofstead filter and a green fluorescent filter upon excitation at both 305 and 365 nm. The fluorescence ceased after the illumination was extinguished; in order to quantify the nature of the fluorescence, a cluster of fibres placed in nanopure deionized water were observed via a Hitachi Fluorometer. When observing the fibers, a characteristic fluorescent pattern emerged: a fluorescent factor (protein) was isolated , and found to have a similar pattern of fluorescence. The cuvette alone did not fluoresce, but an equivalent protein concentration of BSA (bovine serum albumin) gave a fluorescence which differed distinctly from the fibre fluorescence. The fluorescent factor was isolated as a soluble component, and demonstrated to be a molecule of molecular weight greater than 10 kDa. The fluorescence (associated with fibres), isolated to a protein composition, may be a unique feature to Morgellons patients and would greatly assist clinical practicioners in distinguishing between Morgellons and Delusional Parasitosis. Similarly, it may be of interest to survey textile and cellulose fibres for fluorescence, in order to establish the fluorescent fiber hallmark as a unique, non-commercial, non-man-made entity. Further protein analysis of the fluorescent factor may yield clues to the infectious agent identity, as the protein does not correspond to any potential human gene or protein product.
For what concerns internal symptoms, they usually occur as the disease progresses, therefore they will be treated in the apposite section.


(Morgellons disease: Analysis of a population with clinically confirmed microscopic subcutaneous fibers of unknown etiology, 2010)
(Characterization and evolution of dermal filaments from patients with Morgellons disease, 2013)
(Morgellons diagnosis, 2006)
DIAGNOSIS
The diagnosis it's complicated, as no specific agent has been acknowledged to be the trigger of this syndrome; therefore for Morgellons disease, being usually linked to Lyme disease, the most common and most used diagnostic test are for the latter. Looking for Borrelia burgdoferi, the appropriate tests are:
1. Serologic testing
2. PCR fo Bb DNA
3. Co-infection testing
4. CD57 NK testing
5. Spirochete colture
The differential diagnosis should consider and exclude the usual pseudo-scabies, as well as any form of usual bacterial, viral or other fungal infections. Infections with Staphilococcus aureus bacteria can show initially similar symptoms and they may be, sometimes, involved too.
Together with those laboratory tests, visual identification of the subcutaneous protruding filaments and of the skin lesions are the best ways to identify the Morgellons syndrome.

(Characterization and evolution of dermal filaments from patients with Morgellons disease, 2013)
PATHOGENESIS
Starting from the condition described in Symptoms paragraphs, the disease usually develops in two different ways, the first developing and worsening the previous skin condition, the other involving internal organs.
As for the skin, after 6-12 months, alopecia, grey hairs, crusts, erythema and cellulitis are common to be seen; environmental and physical factor can worsen or accelerate the disease.
As the disease proceeds, internal symptoms arise: physical weakness, reduced efficiency, Chronic Fatigue Syndrome with concentration problems, neurological signs and Meningitis or Encephalitis, as well gastrointestinal failure, unexplainable back pain, coughs, rigid neck and other parts, also a generally decreased ocular ability with Keratitis inflammation and a progressive parodontal disease.
Problem is, those symptoms can be caused by Lyme disease, but also by Enteroviruses, EBV, Herpes Simplex 2, HIV (for what concerns viruses), and bacteria like Streptococcus B, Listeria monocytogenes and Enterobacteria.
(Morgellons diagnosis, 2006)
PATIENT RISK FACTOR
Acquired
Apart from the risks that patients may encounter due to the similarity to Lyme disease, the main risk patients undergo is related to the ignorance/reluctance of physician who do not know/do not acknowledge Morgellons as a true disease. The unknown cause and the misguiding sensations reported to the patients (i.e. delusional infestation) may lead physicians to consider it only a dermatological and/or psychological problem.
There is also a risk concerning re-infection because the high rate of survival of spores is in itself a cause of re-infection, which is still possible, even after months of being free from infestation. Even so, unhygienic environments favour the re-infection rate. Disposable clothes, extreme hygiene and discipline are required for a longer time than you might expect to eradicate contagion.

(Morgellons disease: Analysis of a population with clinically confirmed microscopic subcutaneous fibers of unknown etiology, 2010)
(Delusional parasitosis, 2006)
Vascular
Patients often reported orthostatic intolerance and frequent arrhythmias (type undetermined) regardless of age. Rhythm and mild cardiac auscultation abnormalities (valvular) were commonly found on vital sign determination. Pulse was high (>72) in virtually all.
Hormonal
In a study involving 30 patients, eight of them (32%) had prior diagnoses of Hashimoto's Thyroiditis: the U.S. adult prevalence rate of Hashimoto's Thyroiditis is 0.56%. The rate is based on 1996 statistics: 1,490,371 adults with Hashimoto's Thyroiditis per U.S. population of 264,162,000. Half had past evidence of Hypercalcemia (intermittent), of which 3 had definite parathyroid adenomas, later surgically excised with incomplete improvement. Fasting insulin levels were elevated in 100% who were tested for it (6 out of 25), as were CRH levels (also 6 out of 25 tested).
(Morgellons disease, illuminating an undefined illness: a case series, 2009)
TISSUE SPECIFIC RISK FACTOR
Physiopathological
One of the first interested tissue is the skin: the lesions and the fibres obviously compromise skin's protective role, leaving the patients opened to various other infections.
Had the brain been recognised as one of the disease's targets, patients may suffer from Encephalitis and/or Meningitis: the risks are various neurological degenerations up to the destruction of the central nervous system.
If the patient presents keratitis inflammation, he risks to a non-neurological permanent loss of sight; finally, progressive parodontal disease lead to the loss of teeth.
COMPLICATIONS
As this illness concerns both the medical and the psychological aspects of the patients, the complication are to be put on 2 different levels. First, there is the frustration for the disease not to be appropriately recognised and treated: this fact may lead to psychological damages which can further worsen the existing condition. Secondly, there are the tissue permanent lesions: skin, eyes, brain, joints are the main structures that undergo a partial/total loss of function, leaving the patient life-impaired.

THERAPY
Assuming Morgellons disease is linked to Lyme disease ( the most valid theory by now), the treatments are very similar to those Lyme's patients usually undergo. The therapy can be divided in 3 categories:
1. Internal medications, including antibiotics, anti-fungals, anti-virals, anti-parasitics, immune boosters (as patients usually are immuno-compromised) and detoxification treatments
2. Topical treatments, i.e. the equivalent of previous point products adapted to the human skin.
3. Environmental Cleansing treatments, as it is important to avoid a re-infection if the cause lies in the areas frequented by the patients.
(Morgellons diagnosis, 2006)
(Morgellons&Lyme disease treatment overview, 2006)