MDMA (3,4-methylenedioxy-N-methylamphetamine), most commonly known today by the street name Ecstasy, is a semisynthetic member of the amphetamine class of psychoactive drugs, a subclass of the phenethylamines.
Mechanism of action
It is generally thought that the primary relevant pharmacological characteristic of the drug is its affinity for SERTs. SERTs are the part of the serotonergic neuron which remove serotonin from the synapse to be recycled or stored for later use. Not only does MDMA inhibit the reuptake of serotonin into this pump, but it reverses the action of the transporter so that it begins pumping serotonin into the synapse from inside the cell. This protein is also a target of other psychomotor stimulants such as cocaine, amphetamine and methamphetamine.
Moreover other studies show that MDMA acts as a releasing agent of norepinephrine and dopamine besides serotonin. It enters neurons via carriage by the monoamine transporters. Once inside, MDMA inhibits the vesicular monoamine transporter, which results in increased concentrations of serotonin, norepinephrine and dopamine into the cytoplasm and induces their release by reversing their respective transporters through phosphorylation.


Focus on 5-HT1A receptors : Serotonin and psychostimulant addiction
Toxicity
MDMA is considered neurotoxic in humans. The current leading theory is that the metabolism of MDMA-induced dopamine release leads to the lipid peroxidation of serotonergic neurons. This occurs when MAO-B breaks up dopamine into free radicals capable of damaging cells, leading to a reduction in SERTs count and possibly damage or destruction of the axon itself, thus interfering with the integrity of the brain's serotonin network.
It is possible that excess serotonin in the synapse due to MDMA, especially if uses occur within a short period, causes the serotonin cells to produce fewer SERTs, a phenomenon which has already been demonstrated with other serotonin-depleting drugs. MDMA use may also cause a decrease in the number of serotonin receptors on the dendrite of the neuron. See more on Erowid.
A number of studies have demonstrated lasting serotonergic changes occurring due to MDMA exposure.
MDMA users showed decreased global and regional brain 5-HT transporter binding compared with controls. Decreases in 5-HT transporter binding positively correlated with the extent of previous MDMA use.
Other studies have suggested that the brain damage may be at least partially reversible following prolonged abstinence from MDMA.
Former ecstasy users showed a consistent increase in SERT availability in the thalamus, thus ecstasy-induced protracted alterations in the availability of the SERT might be reversible.
However, damage caused by heavy, prolonged use of MDMA may be long lasting (case study).
This study suggests that high-dose MDMA exposure could cause loss of two key protein (serotonin-synthesizing enzyme tryptophan hydroxylase and SERT) markers of brain serotonin neurones, a finding compatible with either physical damage to serotonin neurones or downregulation of components therein.
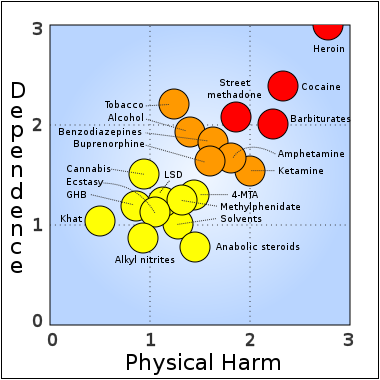 (Lancet)
(Lancet)
Increased doses increase the adverse effects, and some of these (hypertermia, arrhythmias and renal failure) can become life-threatening.
There may be negative long-term consequences that result from the drug's alleged neurotoxic effects on serotonergic neurons: MDMA causes degeneration of serotonin nerve terminals.

Some further studies have also shown that this damage causes increased rates of depression and anxiety, even after quitting the drug. In addition to this, some studies have indicated that MDMA may cause long-term memory and cognition impairment. Many factors, including
- total lifetime MDMA consumption,
- the duration of abstinence between uses,
- the environment of use,
- poly-drug use/abuse,
- quality of mental health,
- various lifestyle choices, and
- predispositions to develop clinical depression and other disorders
may contribute to various possible health consequences.
MDMA use has been occasionally associated with
- liver damage,
- excessive wear of teeth,
- hallucinogen persisting perception disorder (very rarely) .
Marco Lucci Chiarissi, Marco Gastaldo