Fatto da: Giulia Barisone e Giuseppina Ciniglio.
Description
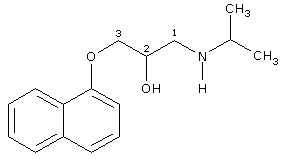
Propranolol is a non selective beta-blocking drug, so it has a moderate affinity for beta 1 and beta 2 receptors. This drug also has a negligible effects at alfa and muscarinic receptors; however it may block some serotonin receptors in the brain, but the clinical significance is unclear.
Indications
Propranolol is used to treat several diseases, in particular for cardiovascular diseases such as hypertension, arrhythmias, angina and in myocardial infarction. It's also used for the treatment of hypertiroidism and thyroiditis, migraine headache, in somatic manifestations of anxiety, in the alcohol withdrawal, portal hypertension and esophageal variceal bleeding, and also used in conjunction with alfa-blocker therapy in phaeochromocytoma.
Classification
Beta-blockers are divided into:
- Non selective
- Selective (for beta 1 or beta 2 receptors)
The first class of drugs includes:
Propranolol,Alprenolol,Bucindolol,Carteolol,Carvedilol,Labetalol,Nadolol,Penbutolol,Pindolol,Timolol. They're non selectives therefore block beta 1 and beta 2 receptors. They're particularly used for the therapy of open-angle glaucoma, headache and myocardial infarction.
The second one,instead,includes: Acebutolol,Atenolol,Betaxolol,Bisoprolol,Celiprolol,Esmolol,Metoprolol,Nebivolol. These drugs have an higher affinity for beta1 than beta 2 receptors and this selectivity leads them to be used for the treatment of CHF,cardiac arrhythmias and myocardial infarction(they're cardioselective). Butaxamine, the only beta-2 selectives antagonist,has no clinical common use.
Atenolol is widely used to treat hypertension. These agents may be safer in patients who experience bronchoconstriction in response to
propranolol. Since their 1 selectivity is rather modest, they should be used with great caution in patients with a history of asthma.
However, in selected patients with chronic obstructive lung disease, the benefits may exceed the risks, in patients with myocardial infarction. Beta1-selective antagonists may be preferable in patients with diabetes or peripheral vascular disease when therapy with a beta-blocker is required since beta2 receptors are probably important in liver(recovery from hypoglycemia)and blood vessels(vasodilation).
Pharmacokinetics
Propranolol is well absorbed after oral administration and undergoes extensive hepatic metabolism (first pass effect). Because of this, its oral bioavailability is relatively low.It is dose-dipendent and seems that the food may increase it. Volume distribution is large: Propranolol has a high lipophilicity so it can pass the blood brain barrier. The metabolism and excretion are due to CYP2D6, an enzyme of the cytochrome P450 present in the hepatocytes.
The half-life of this drug is about 4-6hrs,but its action may last up to 12hrs. Effective plasma concentrations are 10-100ng/ml.
Molecular mechanism
Propranolol binds to beta receptors 1 and 2.
Beta 1 receptor is localized in the miocardium and kidney,while beta 2 receptor is in the vascular's smooth muscle,in the organs' smooth muscle (stomach,bowel,genitourinary tract and bronchi) and also in the skeletal muscle and in liver parenchyma. They're coupled with an adenylate ciclase whick increases cAMP citoplasmatic concentration and then intracellular Calcium.
The block of beta 1 receptor in myocardium determines a decrease in concentration of intracellular calcium which translates in a decrease in cardiac inotropism,cronotropism,dromotropism and batmotropism. According to that mechanism the cardiac output is lower than normal like its work and O2 demand.This is protective for patiences with previous myocardial infarction and for those who have cardiac arrhytmias.Instead the beta1 receptor block in the kidney causes a reduction renin secretion, altough why this happen is unknown.This fact helps in reducing blood pressure.
The block of beta 2 receptor in blood vessels induced an acute rise in peripheral resistance from unopposed alfa-receptor mediated effects as the sympathetic nervous system discharges in response to lowered blood pressure due to the fall in cardiac output. Despite this,however,chronic drug administration leads to a fall in peripheral resistance in patients with hypertension.How this adjustment occurs is not yet clear.Adrenoceptors block is also useful for the treatment of hypertiroidism in which exists an eccessive cathecolamin action,antagonized by Propanolol. Moreover, propranolol and the other beta-blockers with membrane-stabilizing activity, like Alprenolol, decreases plasma T3 concentration and increases rT3. It's possibile that the improvement of signs and symptoms of hypertirodism is due to this mechanism,but it's not proved.
Propranolol and hypertiroidism.
Side effects
Propranolol blocks the activity of beta 1 and beta 2 receptors also in the bronchi, causing bronchospasm and asthma in susceptible patients. Consequently, these drugs should generally be avoided in this patients. Other side effect of this drug is eccessive slowdown of cardiac frequency with an increased risk of hypokinetic arrhytmias and heart failure. This effect is probably due to the fact that in the patients with severe CHF,cardiac output may be dependent on sympathetic drive. If this stimulus is removed by blockade,cardiac decompensation may ensue in some patients, especially with the abrupt discontinuation of the drug. Furthermore,using this drug we can have a rise in blood cholesterol level(because propranolol inhibit sympathetic nervous system stimulation of lipolysis),particularly increased plasma concentrations of VLDL and decreased concentrations of HDL; hypoglicemia in diabetics(because glycogenolysis in human liver is partially inhibited after beta2 receptor blockade).Finally a variety of minor toxic effects have been reported for propranolol: rash,fever and other manifestations of drug allergy are rare. Central nervous system effects include sedation, sleep disturbances and depression.Rarely,psychotic reactions may occur.These last two effects are characteristic of the lipophilic drug like propranolol, that passing the blood brain barrier.
Toxicity
Overdose of Propranolol (plasma concentrations above 2000 ng/ml) may cause seizures, cardiovascular collapse, hypoglycemia, coma and respiratory depression and death. A supportive care includes glucagon infusion and gastric lavage.