DEFINITION
The term Psoriasis refers to an inflammatory disease of the skin, which is simply one of the most common forms of chronic dermatitis in the world.

 Psoriasis
Psoriasis
EPIDEMIOLOGY
Usually chronic and often relapsing, it concerns 1-2% of the world population , including:
- 2% of the population of the United Kingdom;
- 2.6% of the U.S. population;
- In a smaller percentage it affects Japan and West Africa
It affects men and women alike even though there are subtypes of the disease where there is prevalence of one sex. Generally women are to be affected earlier than men, moreover light-skinned individuals are more affected than the ones with darker skin.
SYMPTOMS
The disease occurs more commonly with:
- papules
- erythematous plaques
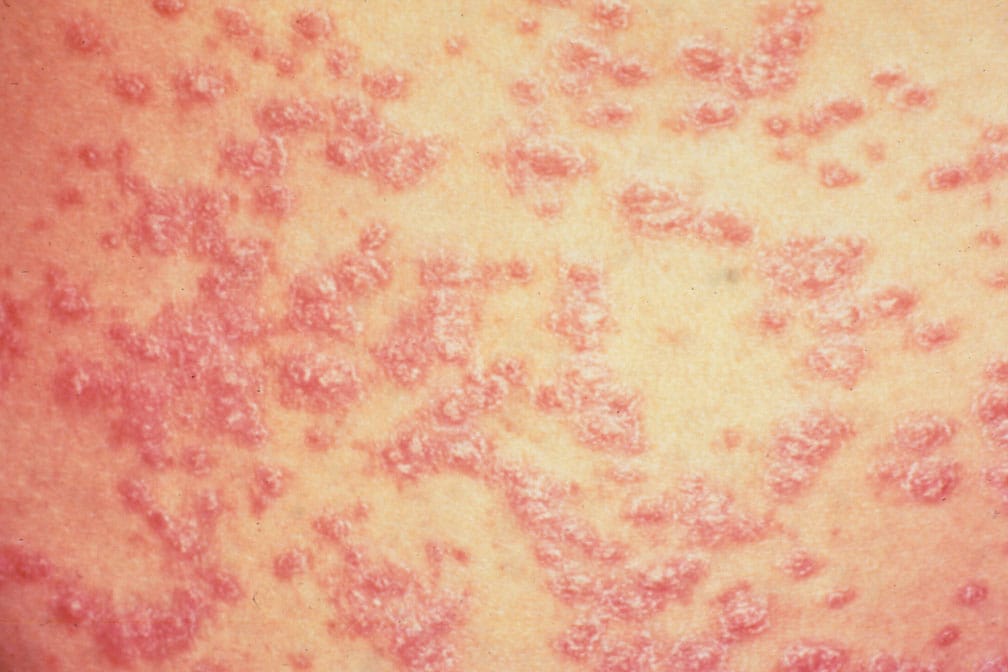

which are red, well demarcated, covered with silvery or opalescent scales.
The lesions vary in size and never affect the mucous membranes. Their diffusion may vary:
- there can be few spots of dandruff type scales, most frequently located at the elbows, knees, scalp and in the navel and sacral areas.
• general dermatosis arthritis (PsA).
• in places where there have been some sorts of physical trauma such as friction, burns, scars etc.. The appearance of lesions of this type, is characteristic, although not exclusive, of psoriasis and is called the Koebner phenomenon (also responsive isomorphism).
DIAGNOSIS
histopathology
radiology
NMR
laboratory tests
PATHOGENESIS
FORMS OF PSORIASIS:
There are different forms of psoriasis:
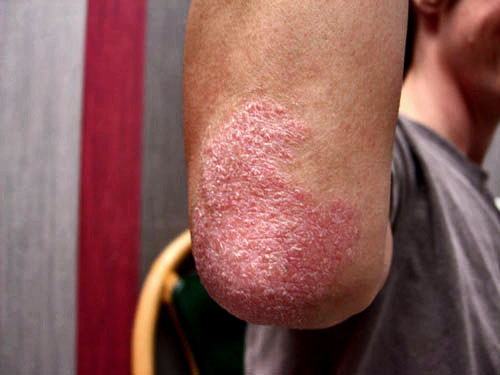
• Plaque psoriasis (psoriasis vulgaris ) ->it accounts for about 80 of all cases of psoriasis . It is a generally mild form of the disease and it affects less than 2 of the body surface area. It shows thickened and reddened plaques slightly larger than one cm round to oval in shape. This form of psoriasis usually affects:
◦ the scalp,
◦ the area below the knee,
◦ the elbow and the forearm
◦ the sacral area.

• Guttate psoriasis -> it accounts for approximately 18% of cases of psoriasis. It most frequently affects children and young adults. Guttate psoriasis is on average a more severe form than plaque psoriasis. It shows small lesions with a diameter ranging from one mm to about one cm. Among the most common factors triggering off psoriasis are tonsillitis and pharyngitis. These lesions, with a characteristic teardrop shape, are located mainly:
◦ on the limbs,
◦ on the face,
◦ on the trunk.

• Pustular psoriasis -> this is a quite rare form of psoriasis (less than 2% of cases), its appearance is usually preceded by other variants of psoriasis. There are two subtypes:
◦ localized pustular psoriasis – the Barber form (the most common type)
◦ generalized pustular psoriasis - the von Zumbusch variant

• Inverted psoriasis -> It is very often linked with plaque psoriasis. It affects with a certain frequency overweight subjects and shows erythematous skin areas, but without scales. The most commonly affected body parts are:
◦ groin,
◦ armpits,
◦ the inframammary fold.
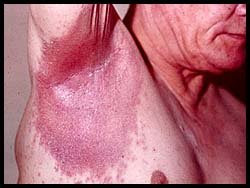
• Erythrodermic psoriasis -> it is a very rare form of psoriasis, but it is certainly the most serious type as it can debilitate the affected individuals in a very severe way and can have complications of considerable gravity. It occurs most frequently in males and the average age of onset is around 50. Usually erythrodermic psoriasis is an evolution of other forms of psoriasis (plaque psoriasis and generalized pustular psoriasis of von Zumbusch).
PATIENT RISK FACTORS
We can have factors triggering psoriasis in predisposed individuals therefore the conditions are defined as triggers. These include:
- Hereditary factors: there is a higher predisposition to be affected by the disease among the children of individuals who have had psoriasis within the age of 30 , together with the other factors mentioned below.
- Emotional stress factors: they are considered important in influencing the history of the disease. In predisposed individuals any event of a certain psycho-emotional relief can worsen the disease or even manifest symptoms until then dormant.
- Medicines: such as lithium (an antidepressant), beta-blockers (antihypertensives), antimalarials, indomethacin, salicylates, iodine compounds can act as triggering factors, while steroids taken by local or systemic way can cause an acute psoriatic rash at the time of suspension or dose reduction.
• Nutrition and lifestyle: even if a direct relationship of alcohol and smoking with the outbreak of psoriasis has not been definitely proven , patients with severe disease are often consumers of alcohol, heavy smokers and have also a diet very rich in animal protein.
• Low intake of omega 3: We know that these essential fatty acids are vital components of biological membranes and the epithelial tissue and contribute to the formation of the hydro-lipid film by the sweat and sebaceous glands in the skin and the scalp. A deficiency of unsaturated fatty acids causes an increase in transepidermal water loss and may be responsible for dry skin, acne and the tendency to develop eczematous states. Numerous studies show that a diet rich in omega-3 from fish oil may have special healthy benefits. In skin diseases such as dermatitis and psoriasis, the composition of the skin sebum undergoes a structural and functional imbalance; in which case the omega-3 helps to restore the percentages of fatty acids ideal for optimal functionality and integrity of the epithelial structure. The use of fatty acids of Omega-3 series helps to balance the fat in blood and the prostaglandins and it has a 'preventive action against the disease. Currently however, new studies have shown that linking the presence of omega3 only to fish is wrong; fish contains only part of the essential fatty acids and in quantities almost non-existent, but the plant world is particularly rich in it, especially in soybean oil, sunflower oil, vegetable oils (flax, hemp, etc. ..), seeds, currants, nuts, dried fruit and pulses, covering the full spectrum of Omega (omega3, Omega6, omega9). Although in smaller quantities omega 3 is also present in the oily fish in the North Sea feeding on plankton, natural salmon, herring, mackerel, swordfish, anchovies, trout, some algae. In addition, the amount of omega-3 polyunsaturated fatty acids contained in many foods depends on the type of preparation: not only cooking but also exposure to sunlight inactivates the essential acid of omega-3 of the food. However, even if the intake of food were rich in omega 3, with age there is a reduction of the denaturasi enzyme, which is Important for the functionality of omega 3. In addition, the diet rich in animal fats, alcohol and adrenaline, cortisol, etc. reduce this enzyme. In shops we can find many products based on of Omega-3; many of these contain Omega-3, Omega-6, Omega-3 precursors mixed with one another or with vitamins. All these compounds belong to the category of dietary supplements.
• Environmental factors: in general the sun and the warm weather improve psoriasis, but sometimes there is a worsening after exposure to sunlight or ultraviolet lamps, especially in light-skinned individuals with photosensitive skin.
Vascular
Genetic
Acquired
Hormonal
Genetic
• Vitamin A: Vitamin A is a liposoluble nutrient that occurs in the natural state in two types: preformed vitamin A and provitamin A or precursor of vitamin A. Retinol is the amount of vitamin A used, which is split up and is in its place in the blood. Beta-carotene is also called precursor or provitamin. This substance is found in fruit and vegetables.
 Psoriasis Vitamin A
Psoriasis Vitamin A
• Vitamin D: Vitamin D is a liposoluble vitamin and can be acquired either by ingestion and with exposure to sunlight. The action of ultraviolet rays activates a form of cholesterol in the skin and converts it into vitamin D. Before becoming active it is altered by the liver and then the kidneys convert it back into its active form, called dihydroxy. Pro-vitamins D are found in animal tissue and plants. A unique aspect of vitamin D is that it behaves like a hormone and so it is sometimes regarded as such, because it prefers organs like the kidneys and intestines. Vitamin D is also used with good results in addition to vitamin A.
 Psoriasis Vitamin D
Psoriasis Vitamin D
• Hormonal factors: the appearance of psoriasis or its exacerbation were found at certain stages of an individual’s life, such as puberty and menopause, therefore suggesting a relationship with the disease.
Acquired
• Metabolic disorders: a state of hypocalcemia (low blood calcium) caused by various causes, including dialysis, is often considered a worsening factor for psoriasis.
TISSUE SPECIFIC RISK FACTORS
anatomical (due its structure)
• Keratinocytes: we have an overproliferation of keratinocytes, which split up about 7-9 times faster than in a normal skin, resulting in alteration of normal turnover. In the epidermis the normal cycle of development, maturation and desquamation of keratinocytes has a duration of about 26 days, whereas in a patient with psoriasis the turnover is reduced to 4 days. The mature keratinocytes go towards the skin surface and accumulate, producing the characteristic scales. You can also check an anomalous development of keratinocytes, which do not fall into the more typical 5 layers. The granular layer is reduced or absent, while the stratum corneum is significantly increased due to the accumulation of keratinocytes. The distribution of various forms of keratin undergoes a change compared to normal skin because of a delay in the development of the basal layer of psoriatic epidermis.
vascular (due to the local circulation)
• T lymphocytes: The psoriatic lesions occur histologically as hyperproliferation areas, with an accelerated epidermal turnover about 10 times faster than the normal skin’s, with an incomplete maturation and maintenance of keratinocyte nuclei in the stratum corneum (parakeratosis), with tortuous neovascularization , increased blood flow, exudation of protein and immature lymphatic vessels; the infiltration of neutrophil polymorphs in the epidermis is to be observed. Even the not affected skin of psoriasis patients shows abnormalities: psoriasis is triggered more easily, especially after a trauma (Koebner phenomenon). The glycogen levels are low compared to the skin of individuals without psoriasis. There seems to be an alteration of cell-mediated immunity(T lymphocytes) and of the epidermal response to certain stimuli. In particular, there seem to be several factors triggering off the dysregulation of T lymphocytes. Other factors probably involved could be the bacterial toxins by-passing the normal control and activating T lymphocytes in an exaggerated way. Another possible cause may be autoimmune factors: a good percentage of psoriasis patients produce antibodies (IgA and IgG) for gliadin, resulting in activation of the lymphocyte response. The pool of activated T cells causes the release of several active substances (γ-interferon, lymphokines). These operate at various levels on the skin, but cannot be solely responsible for the reaction. The psoriatic epidermis is in fact already prepared to an abnormal response: the levels of various substances and the reactivity of tissues to substances normally present are indeed abnormal. Psoriatic skin has high levels of Nerve Growth Factor (NGF), which stimulate the proliferation of keratinocytes. In turn, the keratinocytes release chemokines that further stimulate T cells, thus creating a vicious cycle of self-induced inflammation. It has recently been suggested that to this mechanism, which explains the widespread and chronic inflammation, another one should be added, linked to it, but peculiar to acute injuries. This mechanism involves an active role of infiltration of neutrophils, found precisely within the most acute and active lesions. They are stimulated by chemokines and cytokines released by keratinocytes and T lymphocytes respectively, and in turnthey stimulate the activity of lymphocytes and keratinocytes. A second vicious circle would be therefore created, limited to acute injuries, but still linked to the background inflammation.
References: Pub Med, Treccani, Università degli studi di Roma-La Sapienza
physiopathological (due to tissue function and activity)
- Injury: Various types of trauma are recognized as triggers of the "Koebner phenomenon", since they can lead to psoriatic lesions on apparently healthy skin. These traumatic factors may be of different nature:
- mechanical (abrasion, scratching, injections, insect bites, tattoos, etc.), physical (low temperature)
- chemical (contact with irritant substances)
- other types
- Pyogenic infections: streptococcal infections, especially in the upper respiratory tract in children, often result in the appearance of psoriatic rash or exacerbation of clinical stability. These forms are often more resistant to therapy. Measles often precedes a skin manifestation of psoriasis, but it also often induces an improvement in the course of the disease.
COMPLICATIONS
THERAPY

See the annex about therapy
Alvaro Veronica
Barra Francesca