During pregnancy, the production of steroid hormones greatly increases: at the end, the pregnant woman produces 15-20 mg of estradiol per 24 h, and about 250 mg of progesterone.
This quantity of estrogen is a thousand times higher than that synthesized by a fertile woman, not pregnant. The synthesis of these hormones by the pregnant woman following ways completely different from those followed by a non-pregnant women.
We can say that the placenta plays an important role in the endocrine regulation of pregnancy through the synthesis of hormones, but also through the synthesis of growth factors, neuropeptides and cytokines of various types. The kit of the placenta enzyme, however, is unable to proceed alone to the synthesis of steroid hormones: some enzymatic activities are required by the fetus. The fetal-placental unit, endocrine organ unique to pregnancy, is the result of a biochemical interaction between placental and fetal tissues.

Progesteron and estrogens
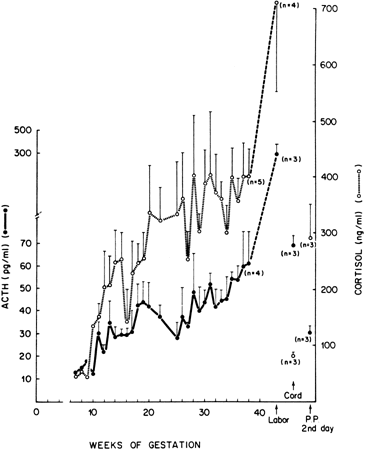
ACTH and cortisol
This picture shows the trend of production of certain during the first months of pregnancy:
Progesterone , 17 alpha OH Progesterone, hCG, estradiol, estrone and estriol.
From the fourth week of gestation the placenta begins to synthesize and secrete progesterone. It is gradually replacing the activity of the corpus luteum gravidarum and shows a steady increase up to term, reflecting the progressive growth of the placenta. After the eighth week, the placenta is the dominant organ in the synthesis of progesterone. In short, the placenta is able to catalyze the reaction that leads to the elimination of the side chain, forming pregnenolone from cholesterol, and the hydroxylation of pregnenolone to progesterone. This is then released into the maternal circulation. A smaller share of progesterone produced by the fetus is derived, but in this case, the pregnenolone sulfate is a precursor. Increased progesterone production is dictated by the fact that this hormone in a pregnant woman warrant endometrial secretion, inhibits the contraction of the myometrium and blocks the maternal immune response. It also prevents other ovulation to occur.
The 17-Alpha-Hydroxy-Progesterone during pregnancy rises slowly until the twelfth week, remains constant up to 32 weeks, and rises again from 32 to 37, probably because it is related to fetal maturation processes.
The placenta lacks the bifunctional enzyme 17alpha hydroxylase /17,20- lyase , and therefore, can’t complete the synthesis of steroid hormones after transforming cholesterol, supplied from maternal blood, into progesterone. To form estrogens through the aromatase enzyme (placenta is rich of this enzyme), the placenta uses the androgens produced by fetus and mother. In detail: the estrogens produced by the placenta are the result of aromatization of androgenic substrates, in turn, produced by the fetus and mother, at the level of the adrenal gland. Among the most common precursors, we recall the DHEA-S, which is produced in equal amounts by the adrenal fetal and maternal. From it derives androstenedione, which is converted into estrone and estradiol . The measurement of these molecules does not reflect accurately the state of fetal well-being, because the substrates are at least half of maternal origin. Much more interesting from this point of view is estriol. DHEA-S produced by the fetal adrenal gland, is converted to 16-hydroxy-DHEA-S from fetal liver, then private of sulfate group by placental sulfatase and then becomes estriol, thanks to placental aromatase. The 16-hydroxy-DHEA-S for 90% derived from fetal tissue and reflects the functioning of the adrenal gland and liver of fetus. Its levels increase gradually, as though by the twentieth week and tripled in the third quarter.This is a typical example of how the placenta relies on the metabolism of mother and fetus, creating an integrated metabolic unit maternal-fetal-placental.
The HCG , human chorionic gonadotropin, is a glycoprotein composed by two subunits. It is produced even before implantation of the blastocyst: its levels show a considerable increase in the first trimester of pregnancy, with a doubling every 48 hours, reaching a peak around the tenth, twelfth week, then a decrease and an adjustment to a much lower level, which is kept constant throughout the rest of the pregnancy. After the first three months of gestation, the HCG level drops because the placenta is now capable of producing by itself a sufficient quantity of hormones. The molecule have been assigned different roles, but certainly the most important is directed at the gestational corpus luteum, where hCG stimulates progesterone production. Other functions are represented by the action on the Leydig cells of fetal testis, where the hCG stimulates testosterone production. HCG also blandly stimulates the maternal thyroid; also helps placenta in the conversion of cholesterol to pregnenolone and progesterone and of estradiol into estriol.


The alphafetoprotein is a glycoprotein synthesized in the yolk sac and in fetal liver in the first three months of pregnancy . Its blood level gradually decrease until it disappears completely at 2-3 weeks after birth.
GnRH is produced by placenta, especially in the first part of pregnancy. Its structure is similar to hypothalamic GnRH.
Identical to pituitary , ACTH is produced by cells of the syncytiotrophoblast and decidua at progressively higher concentrations, up to labor. Its production is modulated by placental CRF. The hormone probably acts in a paracrine way by influencing the placental steroidogenesis and intervening in labor.
IGF-I and IGF-II, insulin like growth factors , are growth factors produced by the trophoblast and later by fetus. They are important in the initial invasion of trophoblast and in the growth of the fetus.
The inhibin and activin modulate the growth and proliferation of various tissues; they are produced by the placenta and fetal membranes, reaching a peak at the end of pregnancy and modulate in different ways the endocrine activity of placenta.
Prolactin is an essential hormone for lactation. It is produced by the maternal hypophysis , the myometrium and endometrio. Prolactin rises between the tenth and the twelfth week, under the stimulus of high levels of estrogen. It then slowly decreases until the end of pregnancy. There is also a prolactin, produced by the decidua, equal to those hypophyseal, whose function is to reduce the permeability of amnios fluids and of electrolytes from fetus to mother.
Endocrinology of Pregnancy at endotext.org
Norma Bocca e Fiorella Maucione