Mononucleosis, also commonly called mono and the kising disease, is an infection most frequently spread through contact with saliva of an infected individual. The disease is caused by an infection by the Epstein-Barr virus, which infects the B-cells of the immune system. The Epstein-Barr virus, also known as EBV and human herpesvirus 4, is a member of the herpesvirus family. As many as 95% of adults in the United States between 35-40 have been infected with EBV at some point in their lives. EBV infections during adolescence have been known to cause infectious mononucleosis 35-50% of the time. It is also known that EBV establishes a lifelong latent infection in the B-cells of the immune system. This latent infection has been linked to Burkitt's lymphoma and nasopharengeal carcinoma. EBV appears to play a role in, but is not the sole cause, of these cancers (Schmid 2005).
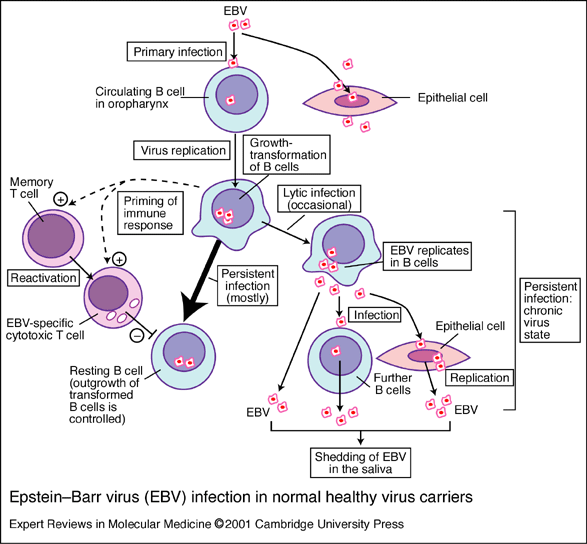
Mononucleosis and the Epstein-Barr virus
Clinical and immunological considerations in Epstein-Barr virus-associated diseases. 1996
Despite the fact that nucleoside analogues, such as aciclovir and ganciclovir, and DNA-polymerase inhibitors, such as foscarnet, have a proven antiviral effect on oropharyngeal-Epstein-Barr virus (EBV) replication, they have been unable to show any effect on the severity or duration of infectious mononucleosis (IM), a condition for which there is currently no established treatment. Clinical symptoms may be due to an EBV-induced polyclonal humoral, as well as cellular, immunoreactivity with limited pathology caused by viral replication itself. However, despite an extensive immune response, 90% of tested IM patients (n = 36) had a spontaneous outgrowth of in vivo EBV-infected B-lymphocytes at onset of disease, indicating lack of specific EBV-restricted cellular cytotoxicity at this time. Establishment of an EBV-specific T-lymphocyte response occurred 90-180 days after onset of disease (human leukocyte antigen-restricted cytotoxicity against EBV-infected B-cells). Thus, development of a specific cytotoxic response was a gradual and slow process. Assessment of cytokine pattern, at the single cell level, was performed by immunocytochemical technique and by enzyme-linked immunosorbent assay. This revealed an increased production of interleukin (IL)-2, interferon (IFN)-gamma, IL-6 and tumour necrosis factor (TNF) beta in all IM patients. Those with disseminated disease were characterized by lack of IFN-gamma production. This loss was selective since in vitro stimulation with superantigen, such as streptococcal pyrogenic exotoxin A, induced a normal response. These patients lacked signs of EBV-specific T-cell cytotoxicity in vitro. Treatment with intravenous or subcutaneous IFN-gamma, 1.5 MU every second day, in combination with intravenous immunoglobulin G (0.5 g/kg three times per week) and oral aciclovir, 800 mg 5 times daily, has shown promising results in some patients. Cytokine production in tonsil tissue in 4 patients with fulminant IM and respiratory tract obstruction showed a concomitant expression of IL-2, IFN-gamma, IL-6, TNF beta, transforming growth factor (TGF) beta 1-3, granulocyte colony stimulating factor, granulocyte macrophage colony stimulating factor, IL-4 IL-1alpha, IL-beta and TNF alpha. The number of IL-2, IFN-gamma, IL-6 and TNF beta producing cells was significantly higher compared to tonsil tissue obtained from children with tonsillar hypertrophy. Thus, IM is associated with extensive local cytokine production. It is suggested that this extensive cytokine production is closely involved in the pathology of IM and that patients with atypical IM have a dysregulation in the cytokine network. However, the mechanism by which EBV-infected B-lymphocytes triggers this cytokine cascade is still unknown. These findings show the need for evaluation of patients with immunodeficiency and EBV-induced lymphoproliferative disorders and perhaps the introduction of new immunoregulatory treatment strategies.
Francesco Delfino - Ceoloni Barbara (Spec. Patologia Clinica)