

Human breast milk is the liquid produced by mammary glands of women after a childbirth ,it should be the first form of nourishment for newborns.
Breastfeeding ist he most common way to give breast milk to the baby who sucks it directly from the nipples.
Production of breast milk
Lactogenesis starts from the twenty-fourth week of pregnancy and involves the change from nonsecretory to secretory state of the epithelial cells of mammmary glands.
The change is influenced by a lot of hormones :
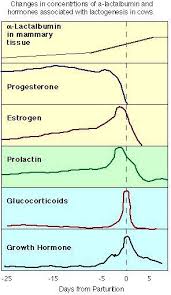 Progesterone
Progesterone
Estrogen
Prolactin
Growth hormone
ACTH and glucocorticoids
TSH
Oxytocin
Human placental lactogen(HPL)
Follicle stimulating hormone(FSH)
Lutenizing hormone (LH)
The maintenance of lactation is called Galactopoiesis and is regulated in part by hormones and in part by local mammary factors.
In this process is fundamental the frequent sucking as this reflexly causes the pituitary gland to secrete prolactin.
To know how lactogenesis works see : mammary glands
or Biology of lactogenenesis
Composition
The composition of breast milk varies from day to day, depending on mother's diet and environment . Breast milk has circadian variations: some of the nucleotides are more commonly produced during the night, others during the day.
There are essentially 3 types of breastmilk :colostrum , foremilk and hindmilk .
Colostrum is the yellowish breastmilk that is produced in the first few days after baby's birth and before normal lactation begins. It is especially rich in nutrients and antibodies that provide passive immunity to the baby . It also helps the newborn's digestive system to grow and function properly.
After 3 or 4 days starts the production of mature milk , during a feeding we have two moments marked by two different type of milk:
The first drawn during a feeding is Foremilk . It is generally thin , watery and lower in fat content , satisfying the baby's thirst and liquid needs . It is rich in proteins, carbohydrates and minerals .
Hindmilk follows foremilk during a feeding. It is creamy , richer in fat content and is high in calories .
During breastfeeding babies must receive both type of milk .
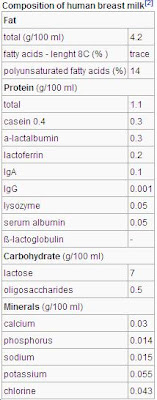 Breastmilk contains all of the nutrients needed by the newborn baby during the first weeks of life. These include the metabolic fuels (fat, protein, carbohydrate), water, and the raw materials for tissue growth and development, such as fatty acids, amino acids, minerals, vitamins, and trace elements.
Breastmilk contains all of the nutrients needed by the newborn baby during the first weeks of life. These include the metabolic fuels (fat, protein, carbohydrate), water, and the raw materials for tissue growth and development, such as fatty acids, amino acids, minerals, vitamins, and trace elements.
More than 98% of the fat in breastmilk is in the form of triglycerides , with comparatively high proportions of the essential fatty acids. High proportions of other long-chain polyunsaturated fatty acids, such as arachidonic acid and docosahexaenoic acid, are also present . These long-chain fatty acids are constituents of brain and neural tissue and are needed in early life for mental and visual development . The lipid component of breastmilk is the transport vehicle for fat-soluble micronutrients such as prostaglandins and vitamins A, D, E, and K.
Proteins account for approximately 75 % of the nitrogen-containing compounds in breastmilk. Non-protein nitrogen substances include urea, nucleotides , free amino acids, and DNA. The principal proteins are casein , alpha-lactalbumin , lactoferrin , IgA, lysozyme, and serum albumin. In an acidic environment such as the stomach, alpha-lactalbumin unfolds into a different form and binds oleic acid to form a complex called HAMLET that is tought to kill tumor cells. This is thought to contribute to the protection of breastfed babies against cancer . Secretory IgA is the principal immunoglobulin of breastmilk.
Many of the proteins in breastmilk have a multitude of potential functions. Lactoferrin, for example, is bacteriostatic and acts as a nutritional protein, producing amino acids for absorption on digestion.
The principal carbohydrate of human milk is lactose, a b-disaccharide manufactured in the mammary epithelial cell . In addition, breastmilk contains significant quantities of oligosaccharides .
In addition to the nutritional components, breastmilk contains a wealth of bioactive components that may have beneficial non-nutritional functions . These include a wide range of specific and non-specific antimicrobial factors ; cytokines and anti-inflammatory substances; and hormones, growth modulators, and digestive enzymes , many of which have multiple activities. Some antimicrobial components are active both within the breast, minimizing the risk of breast infection and mastitis, and within the baby's gastrointestinal and respiratory tracts, protecting the mucosal surfaces from infection by bacteria, viruses, and parasites.
Breastfeeding will normally provide all the nutrient requirements of a baby for the first four to six months of life . After this time some nutrients may become limiting, including not only dietary energy, but also essential minerals such as zinc and iron.
As iron is an essential precursor to the activation of micro-bacteria and gut flora; providing iron in the milk would lead to infection.However, the internal iron supplies of the infant, held in the hepatic cells of the liver, are exhausted at 4–6 months. Current recommendations are that solid foods are unlikely to be necessary before four months, but a mixed diet should be offered by six months .
Moreover, breastmilk can continue to make contributions to infant nutrition for many months after the introduction of weaning foods. This is especially true in communities where weaning and adult foods are of poor quality.
United Nations University Centre- Constituents of Human Milk
Human milk composition,Feb 2013
HAMLET: functional properties and therapeutic potential.2012 Oct
Benefits for the infant
Immune system
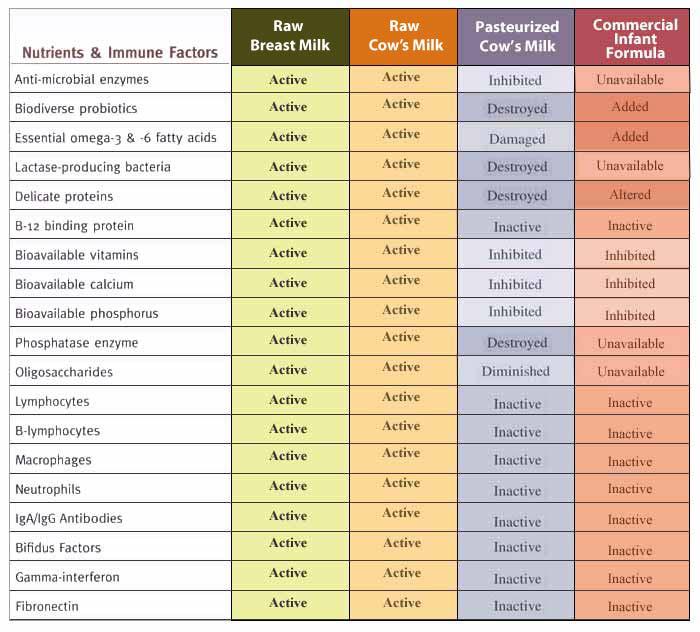 Milk (especially colostrum) offers a form of defence temporary replacement to the baby.
Milk (especially colostrum) offers a form of defence temporary replacement to the baby.
All forms of antibodies have been found in human milk, but the most abundant type is secretory IgA (0.25-0.50 grams per day) .
IgA bind to microorganisms and keep them away from the body’s tissues. Because the mother makes antibodies only to pathogens in her environment, the baby receives the protection it most needs-against the infectious agents it is most likely to encounter in the first weeks of life.
In this way antibodies delivered to the infant ignore useful bacteria normally found in the gut. This flora serves to crowd out the growth of harmful organisms, thus providing another measure of resistance.
Secretory IgA molecules , unlike most other antibodies, ward off disease without causing inflammation . In the Middle East, western South America and northern Africa, women put milk in their infants’ eyes to treat infections there.
Several molecules in human milk besides secretory IgA prevent microbes from attaching to mucosal surfaces.
Oligosaccharides often contain domains that resemble the binding sites through which bacteria gain entry into the cells lining the intestinal tract. Thus, these sugars can intercept bacteria, forming harmless complexes that the baby excretes. In addition, human milk contains large molecules called mucins . They are capable of adhering to bacteria and viruses and eliminating them from the body.
Lactoferrin can bind to iron (used by many bacteria) and disrupts the process by which bacteria digest carbohydrates, further limiting their growth.
Similarly, B12 binding protein deprives microorganisms of vitamin B12. Bifidus factor promotes the growth of a beneficial organism named Lactobacillus bifidus.
Fibronectin, present in large quantities in colostrum, can make certain phagocytes more aggressive so that they will ingest microbes even when they have not been tagged by an antibody. Like secretory IgA, fibronectin minimizes nflammation; it also seems to aid in repairing tissue damaged by inflammation.
Free fatty acids present in milk can damage the membranes of enveloped viruses.
Interferon, found particularly in colostrum has strong antiviral activity.
Several studies indicate that some factors in human milk may induce an infant’s immune system to mature more quickly than it would were the child fed artificially. For example, breast-fed babies produce higher levels of antibodies in response to immunizations. Also, certain hormones in milk (such as cortisol) and smaller proteins (including epidermal growth factor, nerve growth factor, insulinlike growth factor and somatomedin C) act to close up the leaky mucosal lining of the newborn, making it relatively impermeable to unwanted pathogens and other potentially harmful agents. Indeed, animal studies have demonstrated that postnatal development of the intestine occurs faster in animals fed their mother’s milk.
Obesity
There is a connection between the type of postnatal feeding and the development of fat-mass .
Breastfeeding and obesity
SIDS
 Alpha-lactalbumin (LALBA) is the major protein found in breast milk . It is one of the reasons that human milk is superior to cow’s milk in feeding infants . Alpha-lactalbumin has high quantities of several types of amino acids and it has a large amount of tryptophan, which can induce sleep. This amino acid is converted, in the body, to the neurotransmitter serotonin, which can boost moods and lower stress levels . This is why a class of antidepressant drugs acts by increasing serotonin in people suffering from mood disorders . Low levels of serotonine are involved in Sudden Infant Syndrome . In addiction , minor symptoms of infection,especially respiratory tract symptoms, are present in many SIDS cases in the days preceding death, although the illness is not thought to be sufficient to have
Alpha-lactalbumin (LALBA) is the major protein found in breast milk . It is one of the reasons that human milk is superior to cow’s milk in feeding infants . Alpha-lactalbumin has high quantities of several types of amino acids and it has a large amount of tryptophan, which can induce sleep. This amino acid is converted, in the body, to the neurotransmitter serotonin, which can boost moods and lower stress levels . This is why a class of antidepressant drugs acts by increasing serotonin in people suffering from mood disorders . Low levels of serotonine are involved in Sudden Infant Syndrome . In addiction , minor symptoms of infection,especially respiratory tract symptoms, are present in many SIDS cases in the days preceding death, although the illness is not thought to be sufficient to have
caused death, milk with its immunologic properties can help to avoid also these causes .
Intelligence
Numerous studies report that breastfeeding is associated with higher scores on tests of neurodevelopment and cognition in later life , suggesting that breast milk may impact early brain development. These findings are often questioned because other factors associated with mothers’ choice to breastfeed might promote cognitive development .
In all subjects, but most clearly in boys, the effects of breast milk were seen more strongly on white than gray matter in the brain.
In recent years, long-chain polyunsaturated fatty acids (LCPUFAs) have been considered a key explanation for neurodevelopmental benefits of breast milk .
A recent meta-analysis, however, found no conclusive evidence for long-term cognitive effects, suggesting that differences in early LCPUFA intake may not explain our observations.
During the brain development, glial cell production and myelination are key factors related to volume increase.
Breast milk contains significant quantities of cholesterol, it is an indispensable component of myelin membranes and that its availability in oligodendrocytes is a rate-limiting factor in brain maturation.
The massive increase in synapse number postnatally may require large amounts of cholesterol, obtained by neurons from astrocytes .
Serum cholesterol has been related to intellectual performance in adults .
Impact of breast milk on intelligence quotient, brain size, and white matter development, 2010 Apr
Diabetes
Type 1
Type 1 diabetes results from destruction of the insulin-producing ß cells of the pancreatic islets. Various exogenous triggers, such as certain dietary factors and viruses, are thought to induce the immune-mediated process leading to extensive ß cell destruction. Putative mechanisms of protection against type 1 diabetes afforded by breast milk include passive immunity , increased ß cell proliferation observed in breastfed compared with formula-fed infants, or delayed exposure to foreign food antigens in exclusively breastfed infants.In addition, hypotheses have been proposed to explain the putative diabetogenicity of cow milk.For example, ß-lactoglobulin, a cow milk-specific protein, has been implicated as a possible trigger of the immune defect, leading to type 1 diabetes .
Cow's milk exposure and type I diabetes mellitus. A critical overview of the clinical literature. 1994 , Jan
Type 2
Adults and children who develop type 2 diabetes are typically overweight or obese and have a family history of the disease. It is increasingly recognized that nutrition in early postnatal life may have long-term physiologic effects. Studies have suggested that breastfeeding may be protective against later obesity. Therefore, it seems biologically plausible that there may be a relationship between breastfeeding and long-term glucose and insulin metabolism .
Necrotizing Enterocolitis
Necrotizing enterocolitis occurs when the lining of the intestinal wall dies and the tissue falls off.It mostly affects premature infants , involves infection and inflamation. The exact cause of NEC is unknown, but one theory is that the intestinal tissues of premature infants are weakened by too little oxygen or blood flow. So when feedings are started, the added stress of food moving through the intestine allows bacteria normally found in the intestine to invade and damage the wall of the intestinal tissues. The damage may affect only a short segment of the intestine or can progress quickly to involve a much larger portion.
Some experts believe that the makeup of infant formula, the rate of delivery of the formula, or the immaturity of the mucous membranes in the intestines can cause NEC. Babies who are fed breast milk can also develop NEC, but their risk is lower thanks to its immunological action against bacteria and its anti-inflammatory components .
Breast milk and neonatal necrotising enterocolitis. Dec 1990
Other long terms effects
Some studies suggest a connection between breastfeeding and low risk of cardiovascular diseases in later life , as indicated by lower cholesterol and C-reactive protein levels in adult women who had been breastfed as infants. Breastfeeding is also involved in the blood pressure in adults and in stress response but isn't already clear how it works and the results are not confirmed .
Benefits for the mother
Weight Loss
A great deal of research has shown that breastfeeding aids in weight loss. Exclusive breastfeeding can burn up to 500 calories per day, allowing women to get back into their pre-pregnancy clothes even faster compared to women who bottle feed their children. The fat accumulated during pregnancy increases resistance to insulin as well as triglyceride and lipid levels in the blood. Lactation then allows the body to reverse this and enables a woman’s body to return to their normal metabolism after childbirth.
Hormones released and mood
 As prolactin is released from the brain into the mother's bloodstream during breastfeeding, alveolar cells respond by making milk. Oxytocin is the other hormone that plays a vital role because it is necessary for the let-down, or milk-ejection reflex to occur. It stimulates the alveoli cells to contract so the milk can be pushed down into the ducts.
As prolactin is released from the brain into the mother's bloodstream during breastfeeding, alveolar cells respond by making milk. Oxytocin is the other hormone that plays a vital role because it is necessary for the let-down, or milk-ejection reflex to occur. It stimulates the alveoli cells to contract so the milk can be pushed down into the ducts.
Oxytocin also contracts the muscle of the uterus during and after birth, which helps the uterus to get back to its original size and lessens any bleeding a woman may have after giving birth. The release of both prolactin and oxytocin may be responsible in part for a mother's intense feeling of needing to be with her baby .
Prolactin, the milk-making hormone, appears to produce a special calmness in mothers. Breastfeeding mothers have been shown to have a less intense response to adrenaline .
Women who either didn’t breastfeed or stopped breastfeeding early on had an increased risk of postpartum depression .
Oxytocin is often considered the" hormone of love", it is produced naturally in the hypothalamus .
It influences maternal behavior .
Normally brain cells, or neurons, release chemicals such as oxytocin in relatively small amounts from their nerve endings.
But the mother's neurons respond by churning out the hormone from their dendrites - the part of the cell that usually receives, rather than transmits information.
This extra release of oxytocin creates much stronger links between nerve cells - creating a 'positive-feedback' loop, where the greater the concentration of the chemical, the faster it is produced.
Hypothesis of other long-terms benefits for the mother
In these cases the prevention role of breastfeeding in the mother is not fully understood or the results are debatables .
Reduces the risk of breast cancer. Women who breastfeed reduce their risk of developing breast cancer by as much as 25 percent. The reduction in cancer risk comes in proportion to the cumulative lifetime duration of breastfeeding. That is, the more months or years a mother breastfeeds, the lower her risk of breast cancer.
Reduces the risk of uterine and ovarian cancer. One of the reasons for the cancer-fighting effects of breastfeeding is that estrogen levels are lower during lactation. It is thought that the less estrogen available to stimulate the lining of the uterus and perhaps breast tissue also, the less the risk of these tissues becoming cancerous.
Lessens osteoporosis. Non-breastfeeding women have a four times greater chance of developing osteoporosis than breastfeeding women . Because women lose calcium while lactating, some health professionals have mistakenly assumed an increased risk of osteoporosis for women who breastfeed. However, current studies show that after weaning their children, breastfeeding mothers' bone density returns to prepregnancy or even higher levels . In the longterm, lactation may actually result in stronger bones and reduced risk of osteoporosis . Recent studies have confirmed that women who did not breastfeed have a higher risk of hip fractures after menopause .
Benefits child spacing. Since breastfeeding delays ovulation, the longer a mother breastfeeds the more she is able to practice natural childspacing, if she desires. How long a woman remains infertile depends on her baby's nursing pattern .
Breastfeeding and maternal and infant health outcomes in developed countries, 2007 Apr
Unwanted Substances
Breast milk has also been shown to be an excretory route for a range of substances that might be harmful to the baby . These include viruses, such as human immunodeficiency virus (HIV) ; environmental and occupational pollutants, such as DDT , PCBs , and dioxins ; components of the mother's diet that might be toxic or allergenic, such as trans-fatty acids , aflatoxins, and cow's milk protein ; commonly used stimulants, such as nicotine, caffeine, and theobromine ; and various drugs and radioactive compounds .